Содержание
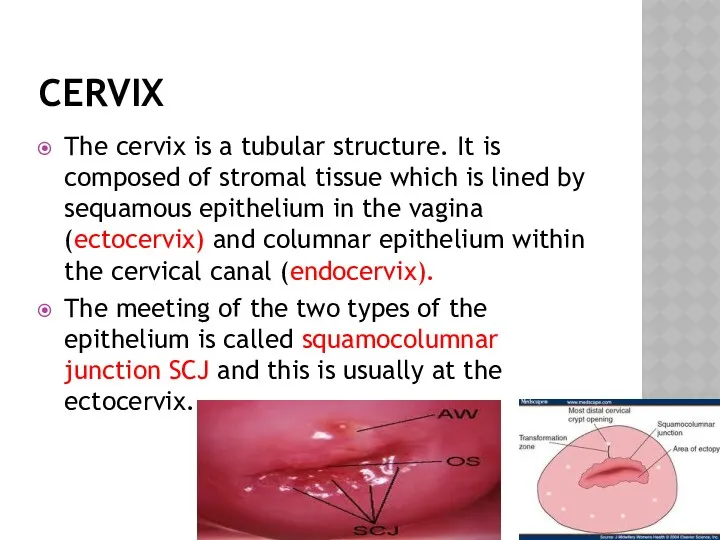
- 2. CERVIX The cervix is a tubular structure. It is composed of stromal tissue which is lined
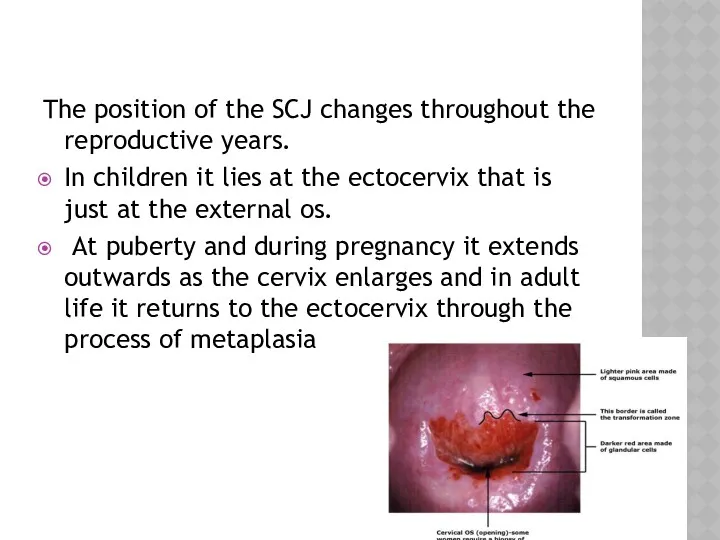
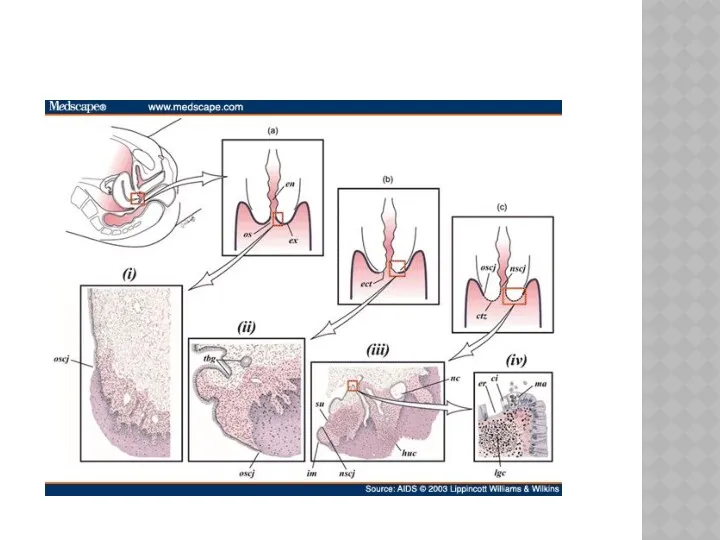
- 3. The position of the SCJ changes throughout the reproductive years. In children it lies at the
- 4. TRANSFORMATION ZONE: is an important area on the cervix which is defined as the area where
- 5. DEFINITIONS AND TERMINOLOGY: CIN: cervical intraepithelial neoplasia, Dysplasia: a histological term describing architectural abnormalities within the
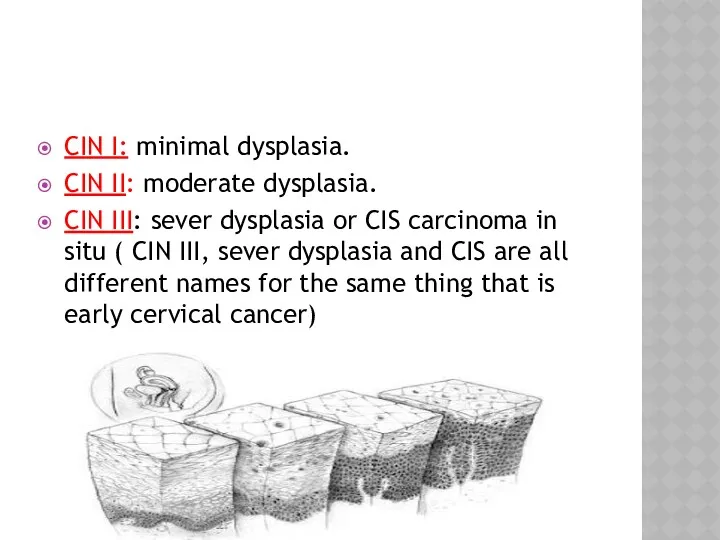
- 6. CIN I: minimal dysplasia. CIN II: moderate dysplasia. CIN III: sever dysplasia or CIS carcinoma in
- 7. Metaplasia: a physiological process whereby columnar epithelium is replaced by squamous tissue in response to the
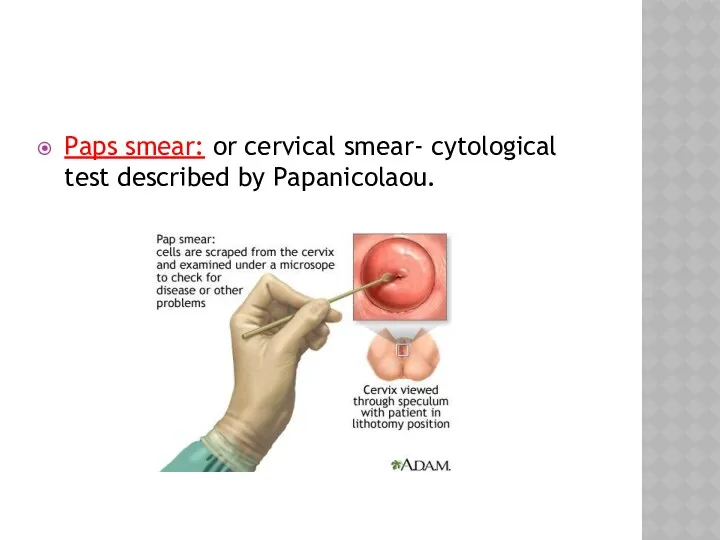
- 8. Paps smear: or cervical smear- cytological test described by Papanicolaou.
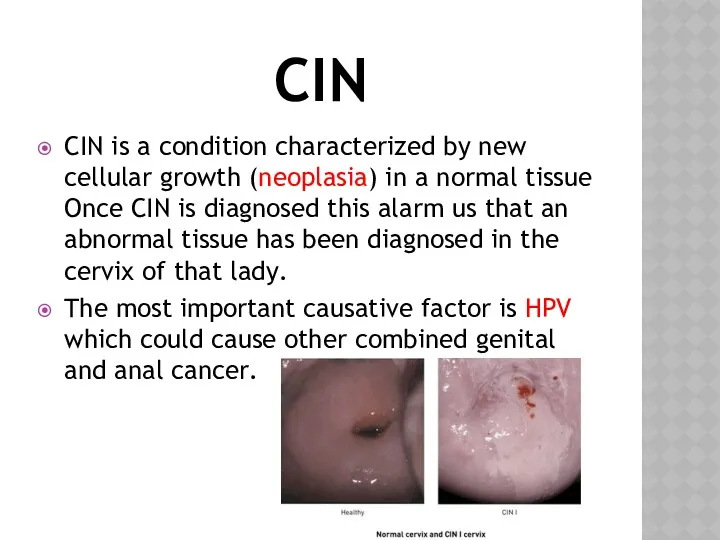
- 9. CIN CIN is a condition characterized by new cellular growth (neoplasia) in a normal tissue Once
- 10. However, CIN is much more common than the other types of genital neoplasia. The tissue changes
- 11. CLASSIFICATION OF CIN: A revised classification has been introduced: Low – grade lesion CIN I and
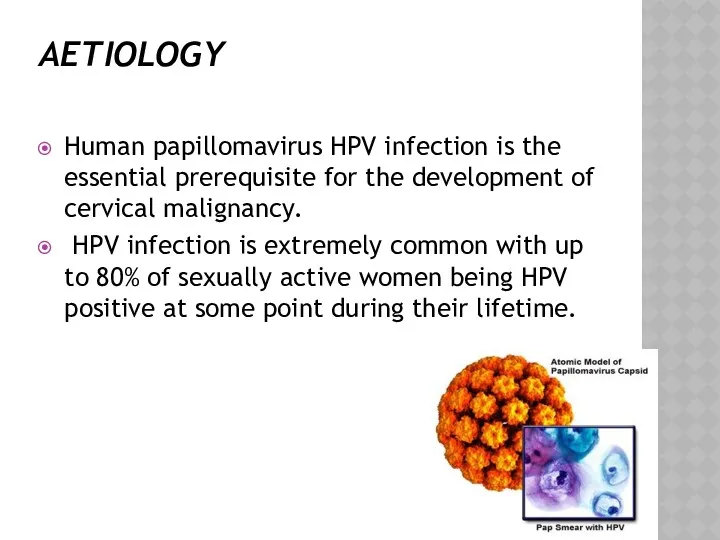
- 13. AETIOLOGY Human papillomavirus HPV infection is the essential prerequisite for the development of cervical malignancy. HPV
- 14. Using the incidence of genital wart as a marker, the incidence appears to be raising five
- 15. RISK FACTORS Smoking reduces local cervical immunity. Multiple sexual partners. Having a partner with multiple sexual
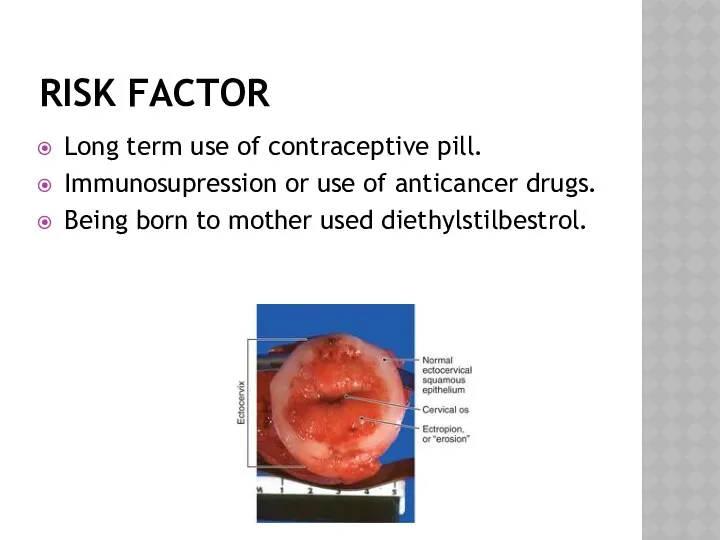
- 16. RISK FACTOR Long term use of contraceptive pill. Immunosupression or use of anticancer drugs. Being born
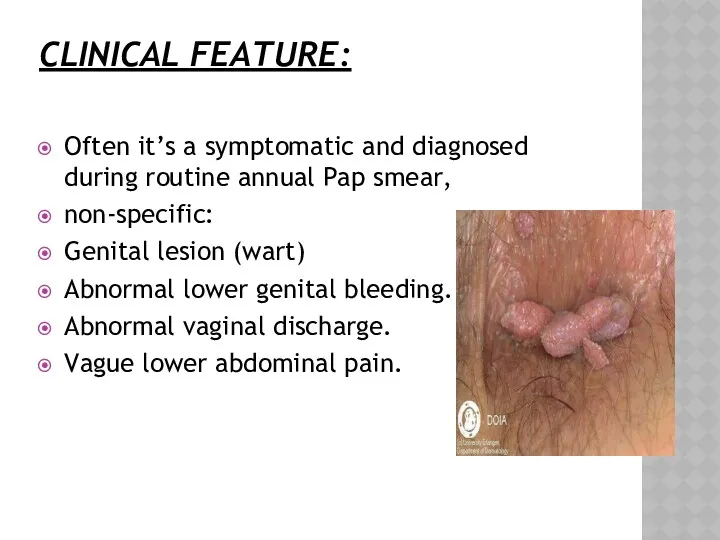
- 17. CLINICAL FEATURE: Often it’s a symptomatic and diagnosed during routine annual Pap smear, non-specific: Genital lesion
- 18. PATHOPHYSIOLOGY: Metaplasia is a normal finding but this may be disrupted by some factors like HPV,
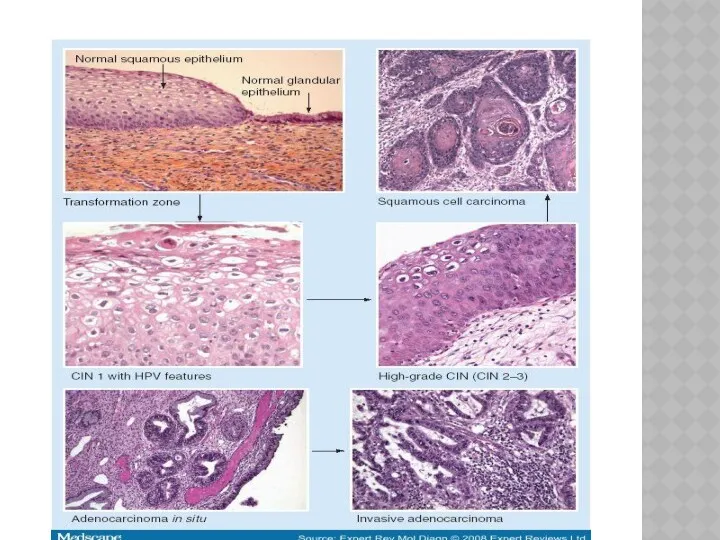
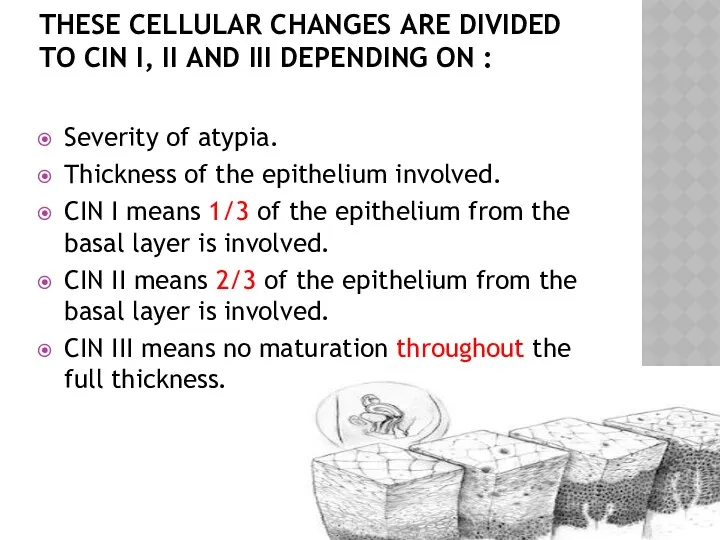
- 20. THESE CELLULAR CHANGES ARE DIVIDED TO CIN I, II AND III DEPENDING ON : Severity of
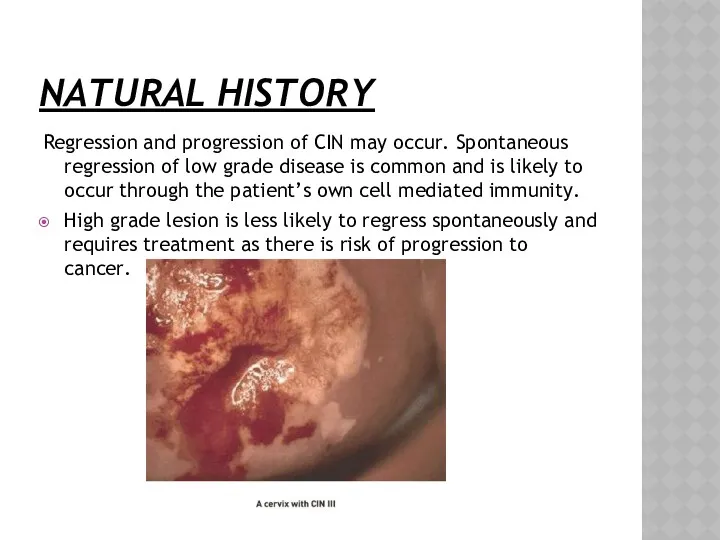
- 21. NATURAL HISTORY Regression and progression of CIN may occur. Spontaneous regression of low grade disease is
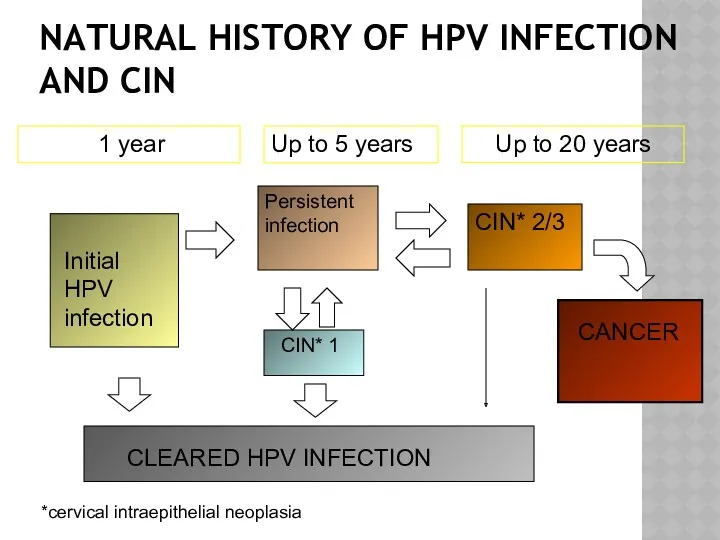
- 22. NATURAL HISTORY OF HPV INFECTION AND CIN Initial HPV infection CLEARED HPV INFECTION CIN* 1 Persistent
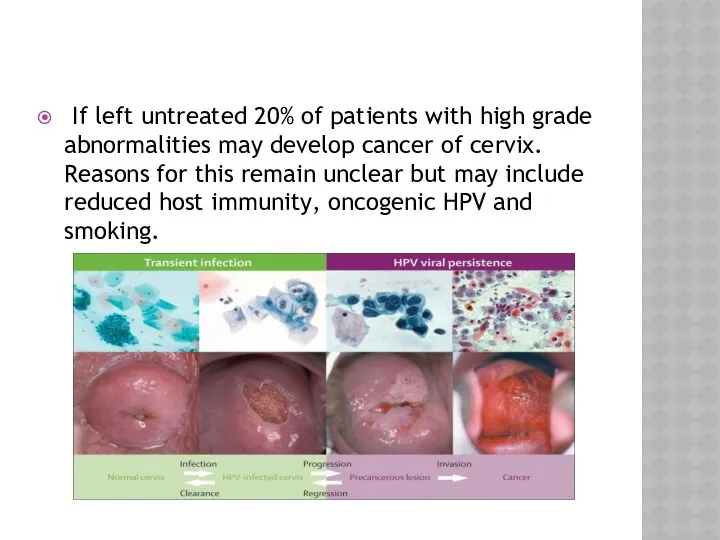
- 23. If left untreated 20% of patients with high grade abnormalities may develop cancer of cervix. Reasons
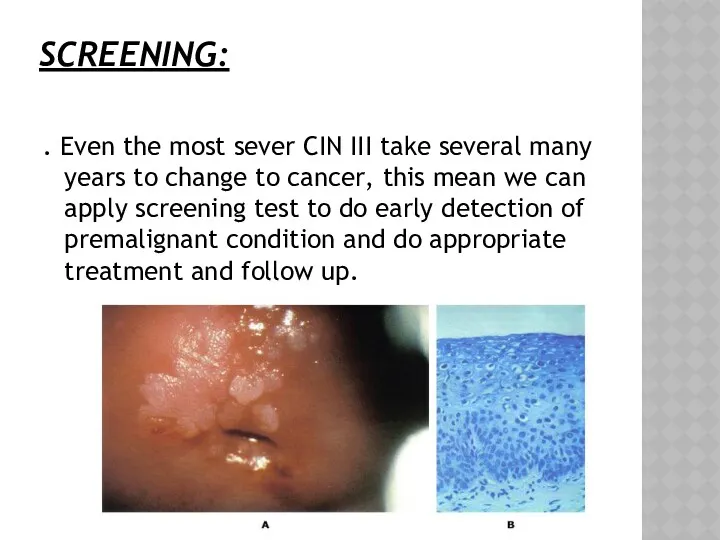
- 24. SCREENING: . Even the most sever CIN III take several many years to change to cancer,
- 25. SCREENING IS DONE BY USING PAP CYTOLOGICAL TEST Since 1988, the UK has offered population based
- 26. TEST PERFORMANCE: Originally the “Pap” smear was introduced by Papanicolou, where cell removed from the cervix
- 27. Now Pap smear is superseded by liquid based cytology where a small brush is used to
- 28. An abnormal smear can show cells in different degree of maturity (dyskaryosis) and is divided into:
- 29. The sensitivity of cervical smear in picking up women with CIN is around 70 percent, however,
- 30. If the smear shows low grade changes the patient offered repeated test in next 3-6 months
- 31. TECHNIQUE OF SMEAR: Patient in lithotomy position under good light, start by inspection (spread labia and
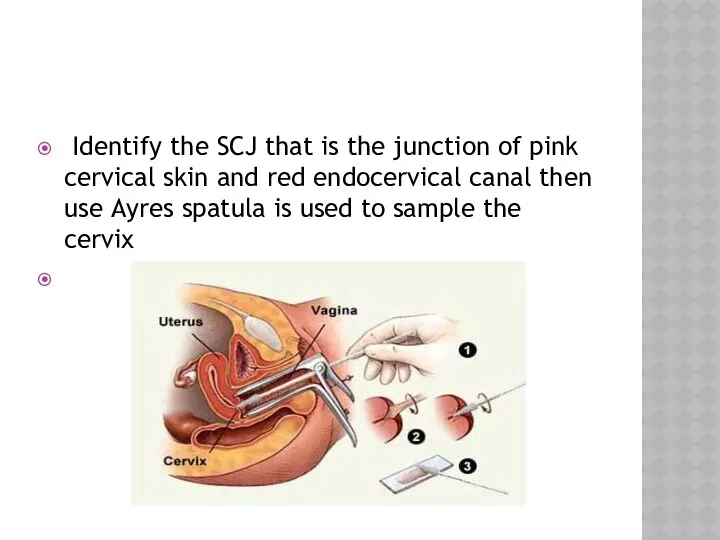
- 32. Identify the SCJ that is the junction of pink cervical skin and red endocervical canal then
- 33. the concave end is used to fit the cervix and should be rotated 360 degree do
- 34. COLPOSCOPY: Colposcopy is the outpatient examination of the magnified cervix using a light source. It is
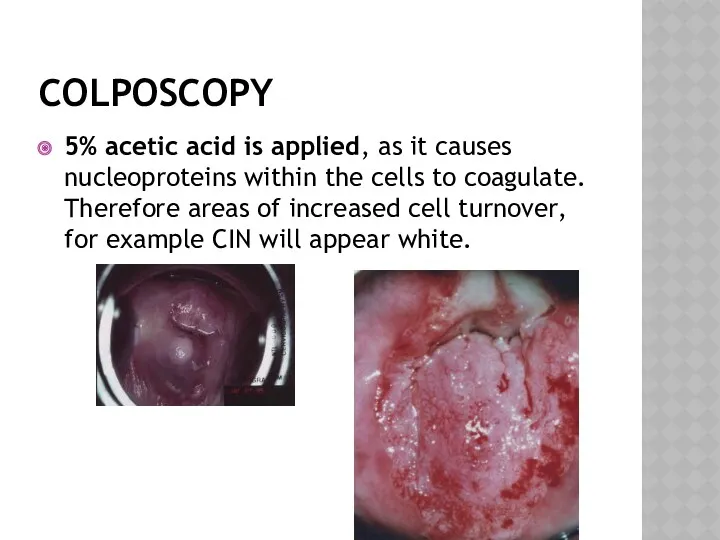
- 35. COLPOSCOPY 5% acetic acid is applied, as it causes nucleoproteins within the cells to coagulate. Therefore
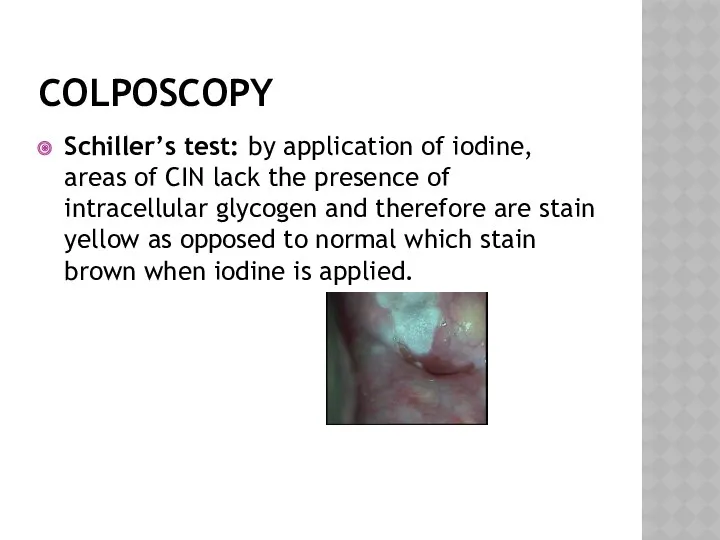
- 36. COLPOSCOPY Schiller’s test: by application of iodine, areas of CIN lack the presence of intracellular glycogen
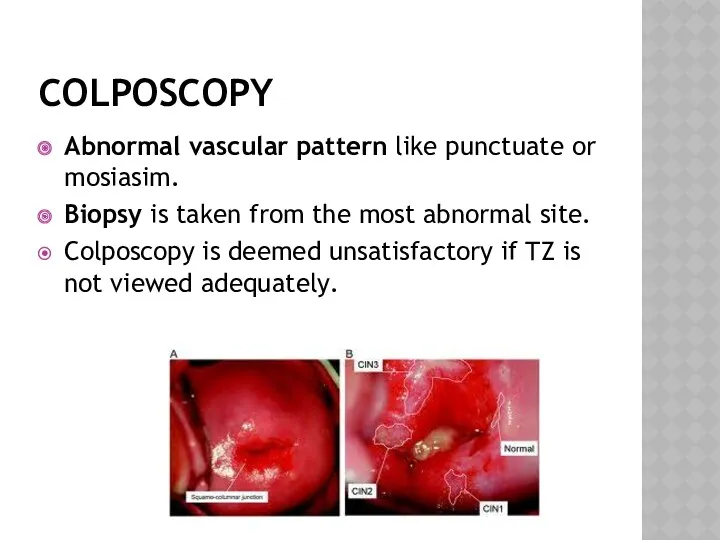
- 37. COLPOSCOPY Abnormal vascular pattern like punctuate or mosiasim. Biopsy is taken from the most abnormal site.
- 38. HPV DNA TESTING: As HPV is the main causative factor of CIN and cervical cancer, recently
- 39. TREATMENT OF CIN: The aim of treatment is to make the post- treatment test negative while
- 40. TREATMENT Could be out patient or in patient Excisional methods like: Loop electrosurgical excision (LEEP) and
- 41. Ablative methods: Cryocautery. Electrodiathermy Coagulation Laser.
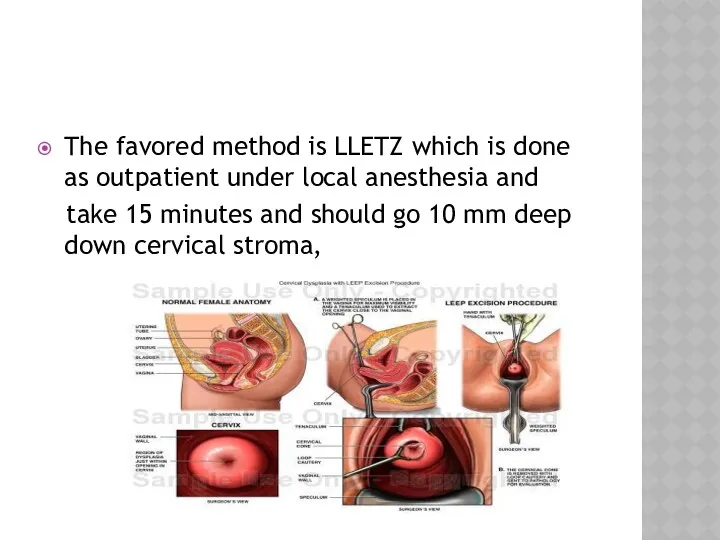
- 42. The favored method is LLETZ which is done as outpatient under local anesthesia and take 15
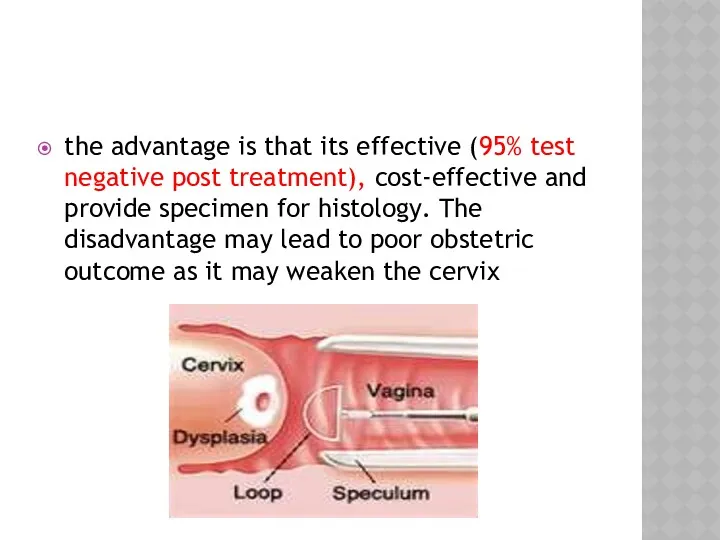
- 43. the advantage is that its effective (95% test negative post treatment), cost-effective and provide specimen for
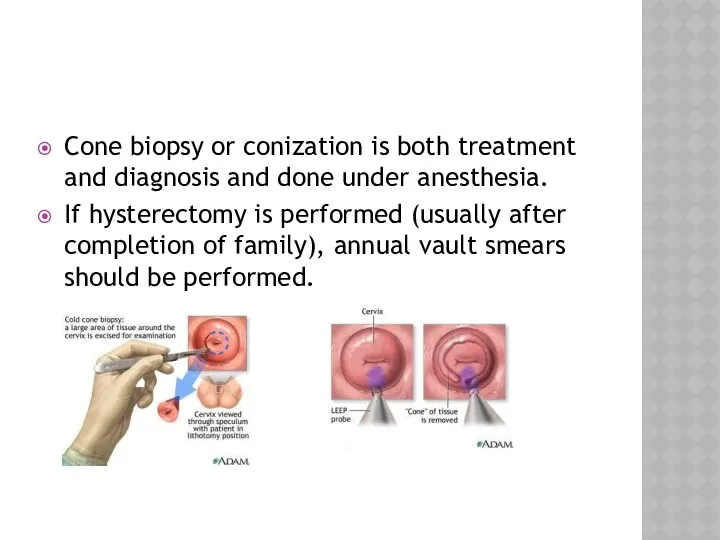
- 44. Cone biopsy or conization is both treatment and diagnosis and done under anesthesia. If hysterectomy is
- 45. FOLLOW UP: Close follow up after initial treatment by regular cervical smear is needed after six
- 47. Скачать презентацию






















 Перспективы генной инженерии человека
Перспективы генной инженерии человека Стеклянная лягушка
Стеклянная лягушка Тип Членистоногие
Тип Членистоногие сон и сновидения
сон и сновидения Стійкість рослин до несприятливих умов середовища. Види стійкості
Стійкість рослин до несприятливих умов середовища. Види стійкості Лекарственные растения
Лекарственные растения Бактерии. Автотрофы и гетеротрофы. Значение бактерий в жизни человека
Бактерии. Автотрофы и гетеротрофы. Значение бактерий в жизни человека Тест по биологии (8 класс) по теме Биосоциальная сущность человека для системы тестирования PROClass
Тест по биологии (8 класс) по теме Биосоциальная сущность человека для системы тестирования PROClass Селекцiя
Селекцiя Мейоз
Мейоз Интересные животные и растения Африки
Интересные животные и растения Африки Ознаки захворювань капусти білоголової
Ознаки захворювань капусти білоголової Несъедобные и ядовитые грибы
Несъедобные и ядовитые грибы Биополимеры. Углеводы. Липиды
Биополимеры. Углеводы. Липиды Предшественники человека
Предшественники человека Химический состав клетки
Химический состав клетки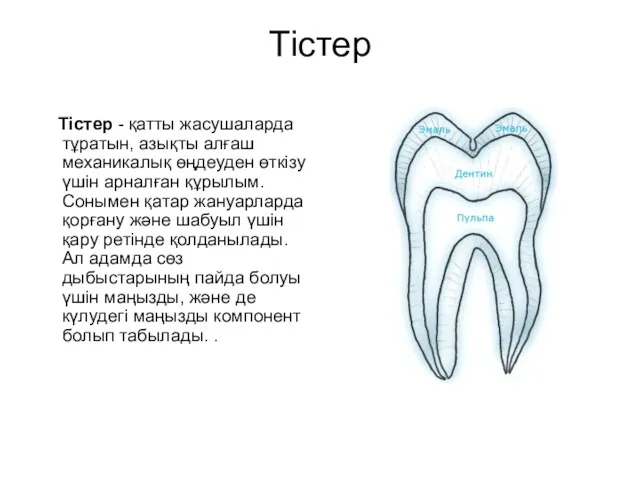 Тістер. Сүт тістер
Тістер. Сүт тістер Водоросли, 5 класс
Водоросли, 5 класс 09_02_biologia
09_02_biologia Среды жизни и места обитания животных. Взаимосвязи животных в природе
Среды жизни и места обитания животных. Взаимосвязи животных в природе Молочнокислые бактерии
Молочнокислые бактерии Биология. 5 класс. Тесты
Биология. 5 класс. Тесты Плауны. Хвощи. Папоротники
Плауны. Хвощи. Папоротники Сырдарияның гидробиологиялық режимі
Сырдарияның гидробиологиялық режимі Динозавры (ужасные ящеры)
Динозавры (ужасные ящеры) Стандартизация растениеводческой продукции
Стандартизация растениеводческой продукции Генетичний алгоритм
Генетичний алгоритм Ара шаруашылығындағы азық қоры
Ара шаруашылығындағы азық қоры