Содержание
- 2. Background Total joint replacement is one of the most commonly performed and successful operations in orthopaedics
- 3. Background Total joint replacement (TJR) is one of the most cost-effective procedures in all of medicine.
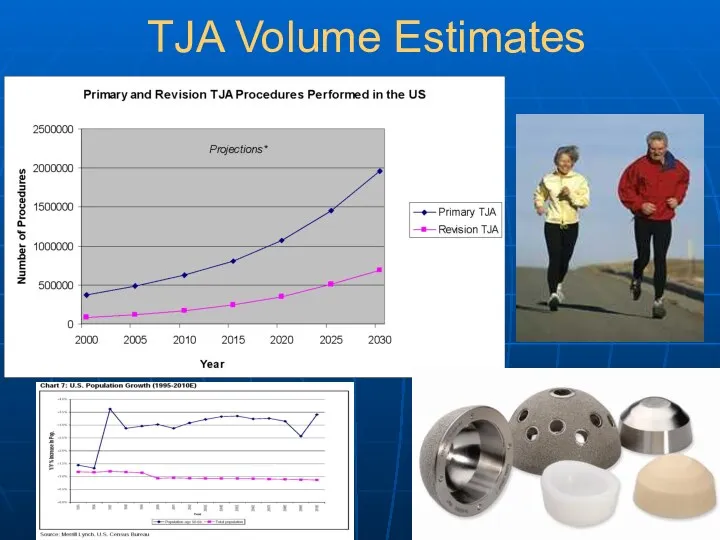
- 4. TJA Volume Estimates
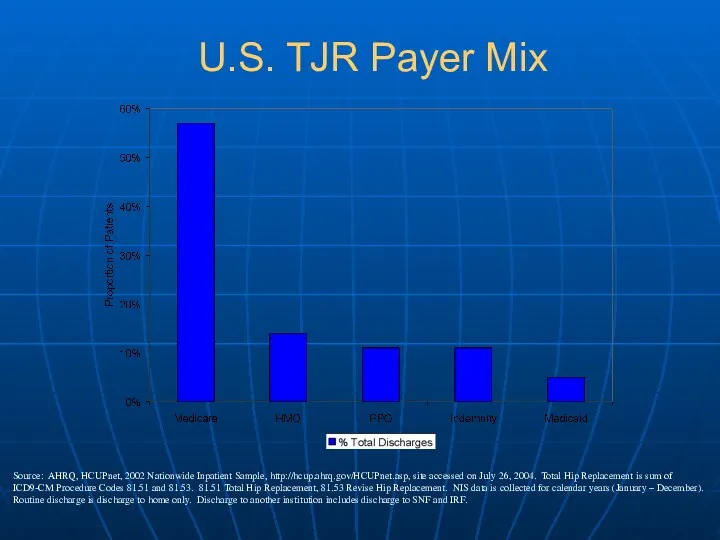
- 5. Source: AHRQ, HCUPnet, 2002 Nationwide Inpatient Sample, http://hcup.ahrq.gov/HCUPnet.asp, site accessed on July 26, 2004. Total Hip
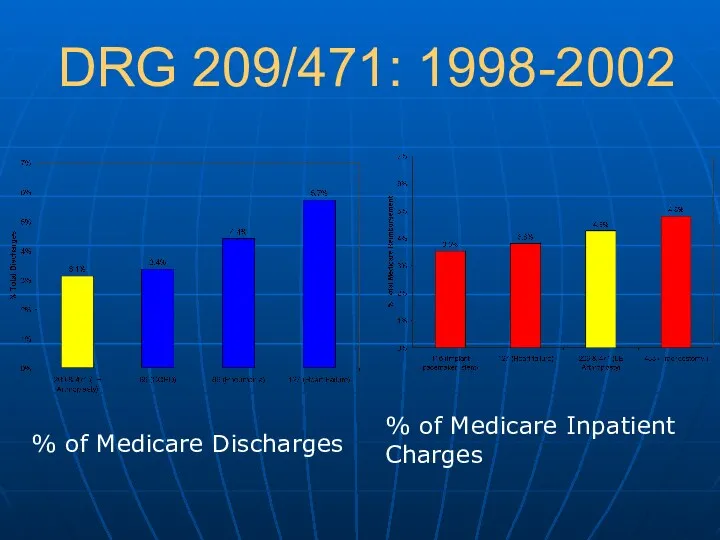
- 6. DRG 209/471: 1998-2002 % of Medicare Discharges % of Medicare Inpatient Charges
- 7. TJR Failure Despite the success achieved with most primary TJR procedures, factors related to implant longevity
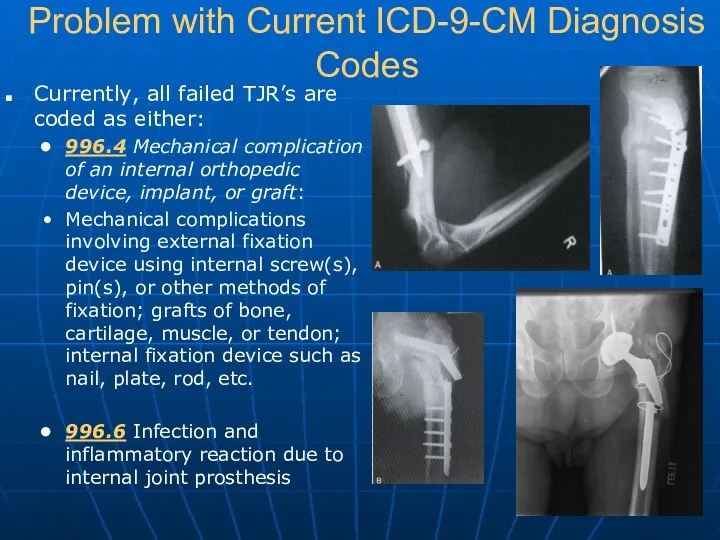
- 8. Problem with Current ICD-9-CM Diagnosis Codes Currently, all failed TJR’s are coded as either: 996.4 Mechanical
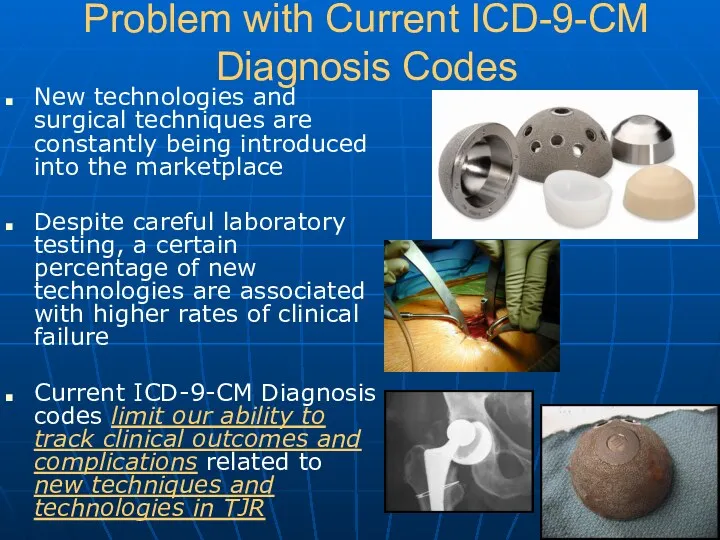
- 9. Problem with Current ICD-9-CM Diagnosis Codes New technologies and surgical techniques are constantly being introduced into
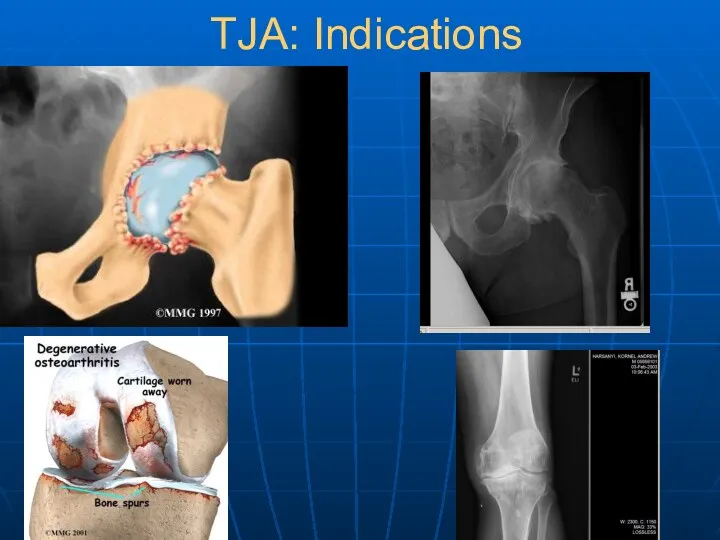
- 10. TJA: Indications
- 11. Arthritis—Background Arthritis is the second most common chronic condition in the US (sinusitis is first) Most
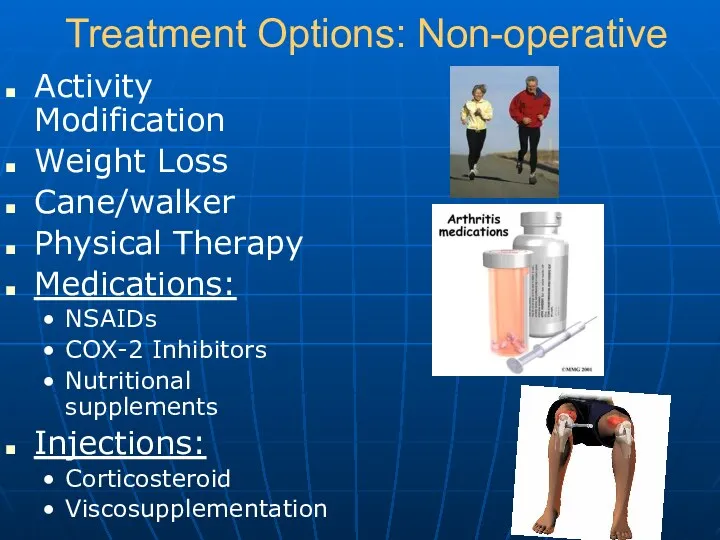
- 12. Treatment Options: Non-operative Activity Modification Weight Loss Cane/walker Physical Therapy Medications: NSAIDs COX-2 Inhibitors Nutritional supplements
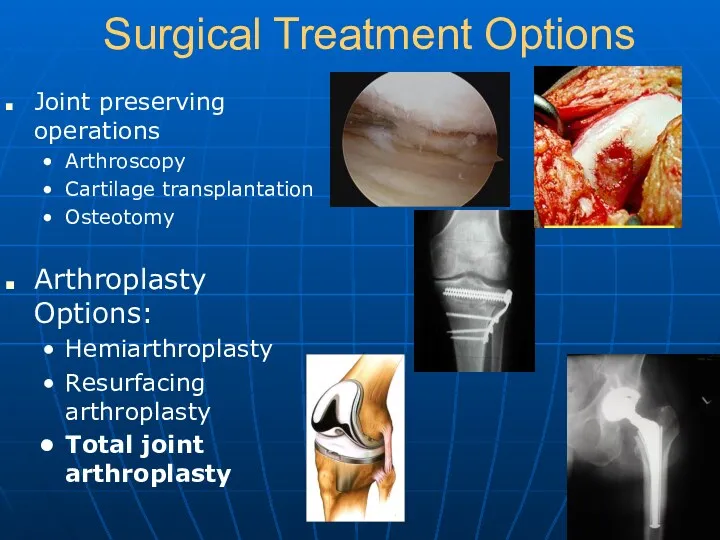
- 13. Surgical Treatment Options Joint preserving operations Arthroscopy Cartilage transplantation Osteotomy Arthroplasty Options: Hemiarthroplasty Resurfacing arthroplasty Total
- 14. Goals of Joint Replacement Surgery Relieve pain!!! Restore function, mobility
- 15. Anatomy—Hip
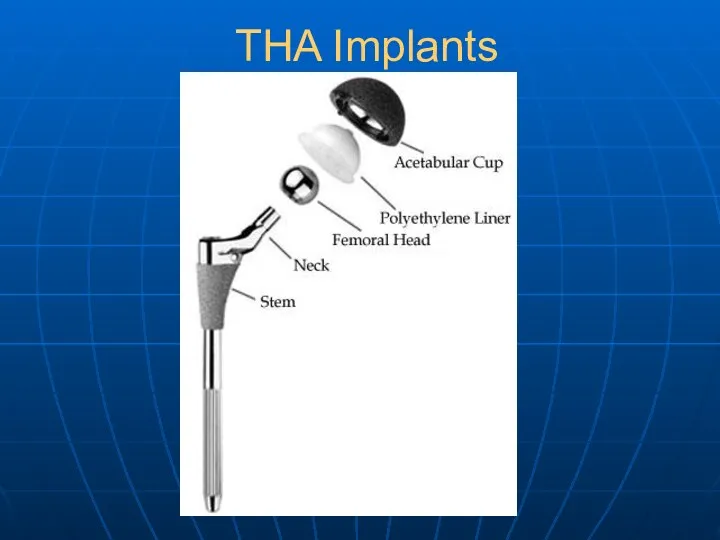
- 16. THA Implants
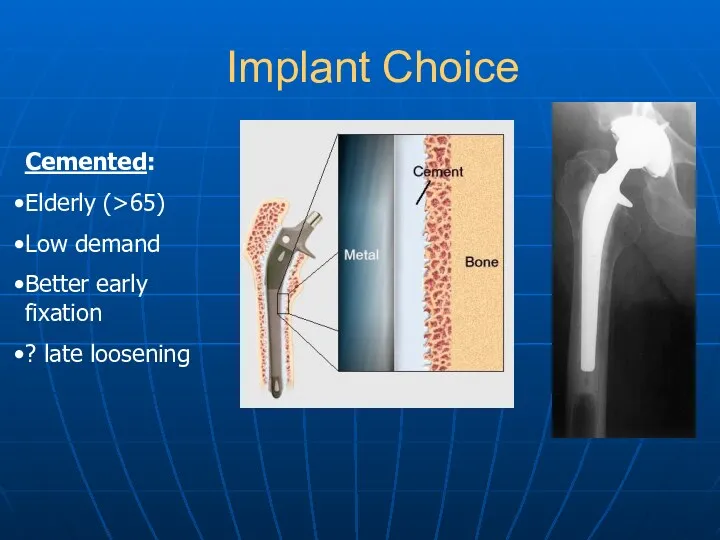
- 17. Implant Choice Cemented: Elderly (>65) Low demand Better early fixation ? late loosening
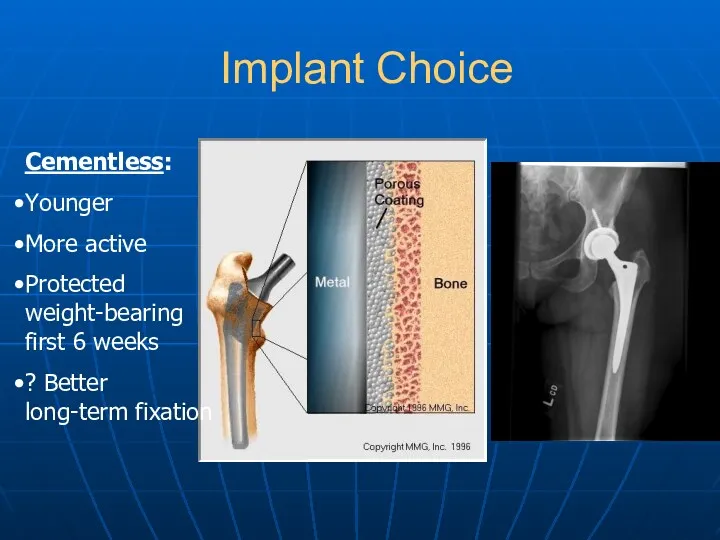
- 18. Implant Choice Cementless: Younger More active Protected weight-bearing first 6 weeks ? Better long-term fixation
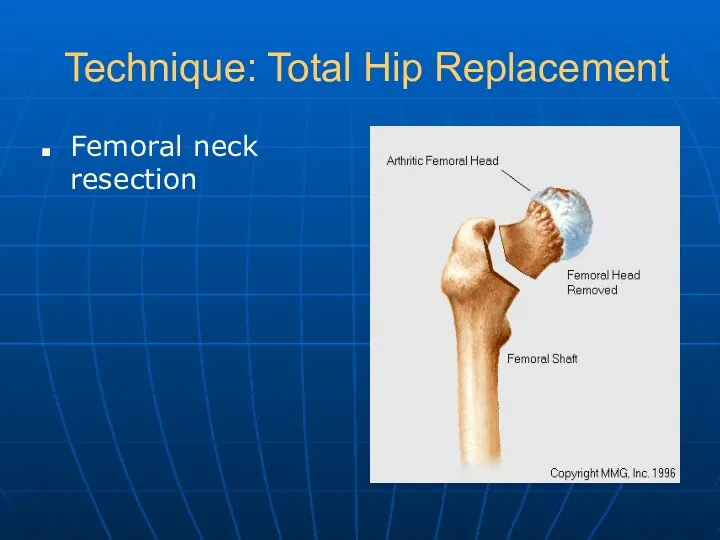
- 19. Technique: Total Hip Replacement Femoral neck resection
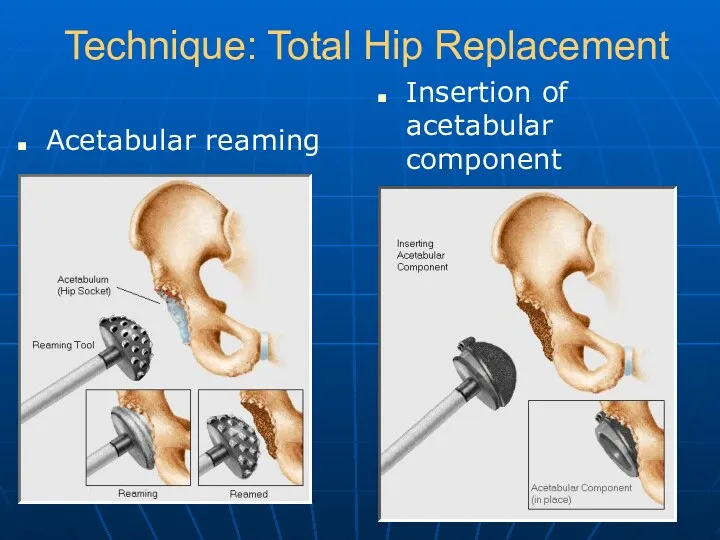
- 20. Technique: Total Hip Replacement Acetabular reaming Insertion of acetabular component
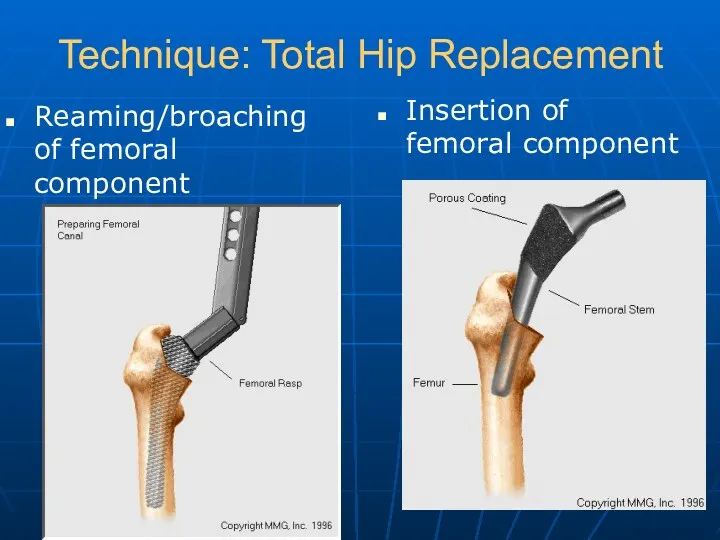
- 21. Technique: Total Hip Replacement Reaming/broaching of femoral component Insertion of femoral component
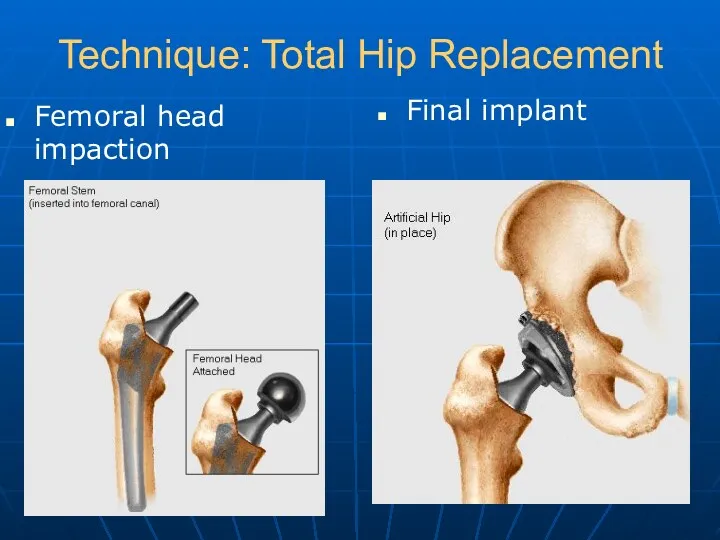
- 22. Technique: Total Hip Replacement Femoral head impaction Final implant
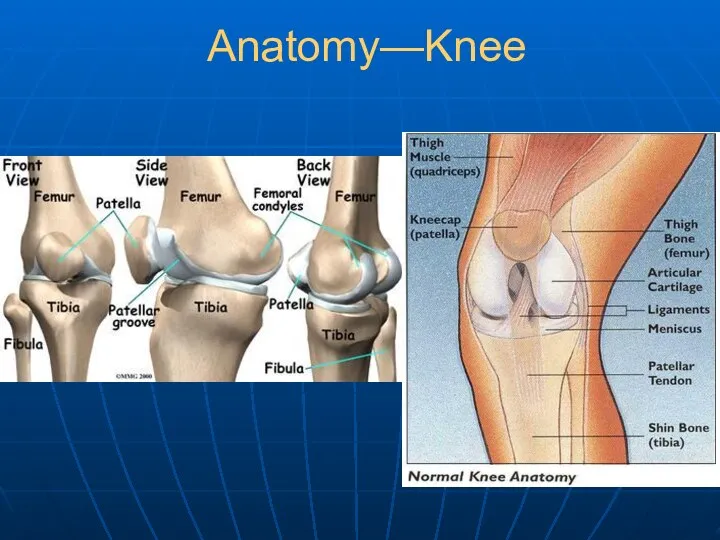
- 23. Anatomy—Knee
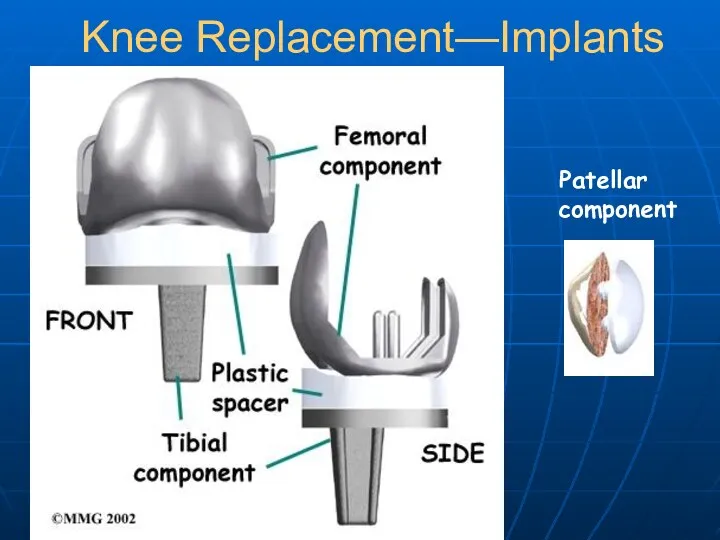
- 24. Knee Replacement—Implants Patellar component
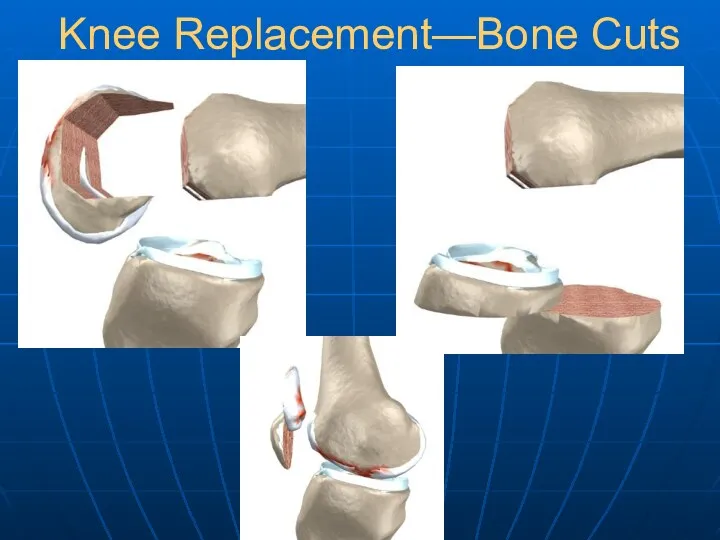
- 25. Knee Replacement—Bone Cuts
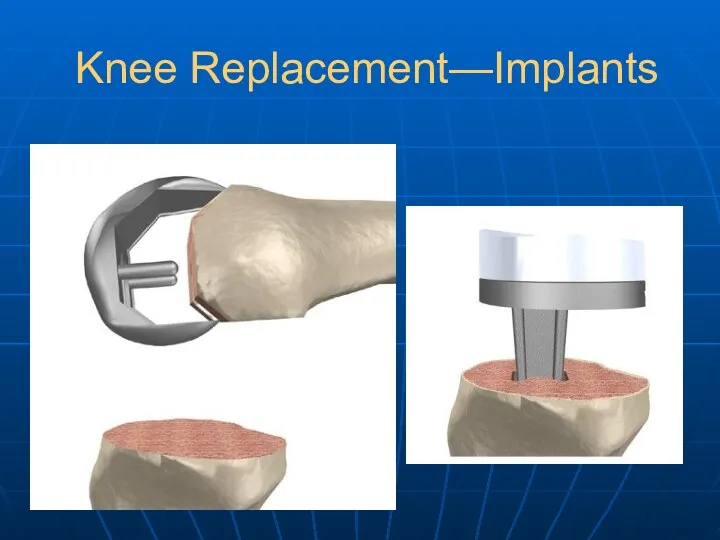
- 26. Knee Replacement—Implants
- 27. Knee Replacement—Implants
- 28. Causes of TJR Failure Wear of articular bearing surface Aseptic/mechanical loosening Osteolysis Infection Instability Peri-prosthetic fracture
- 29. Timing of TJR Failure Early ( Dislocation Infection Implant failure Late (> 5 yrs post op)
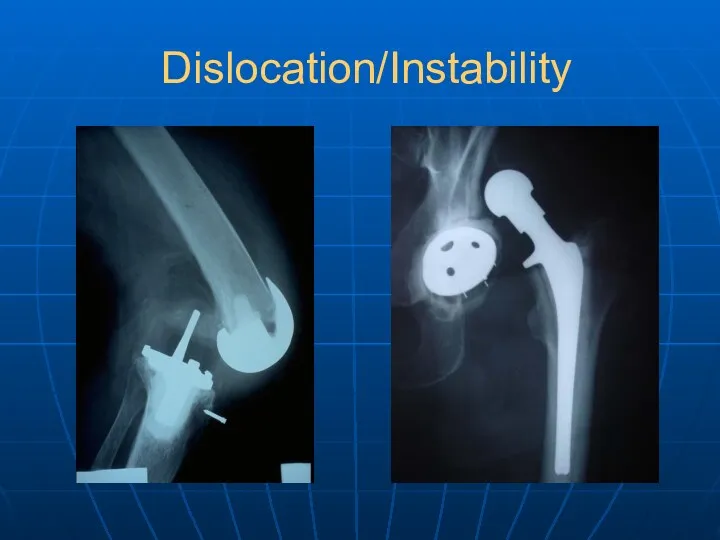
- 30. Dislocation/Instability
- 31. Infection
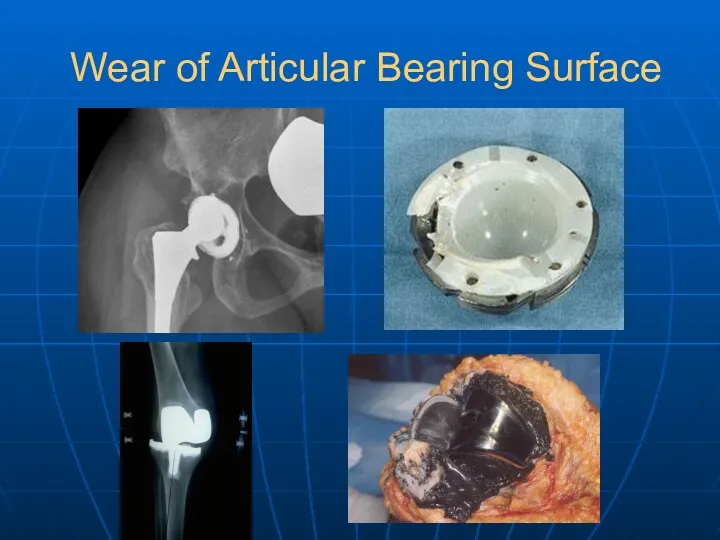
- 32. Wear of Articular Bearing Surface
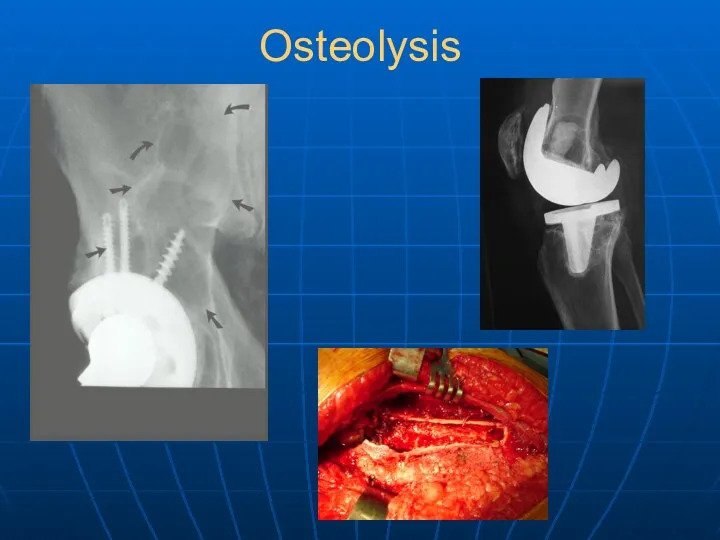
- 33. Osteolysis
- 34. Aseptic/Mechanical Loosening
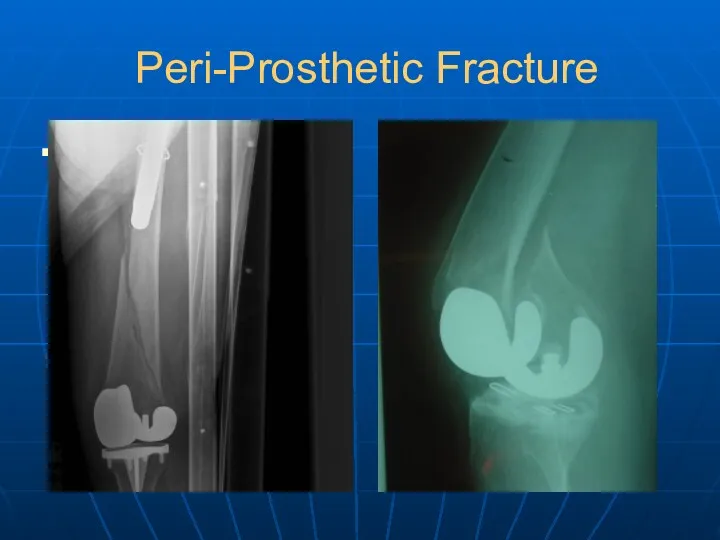
- 35. Peri-Prosthetic Fracture Sri: PP fracture
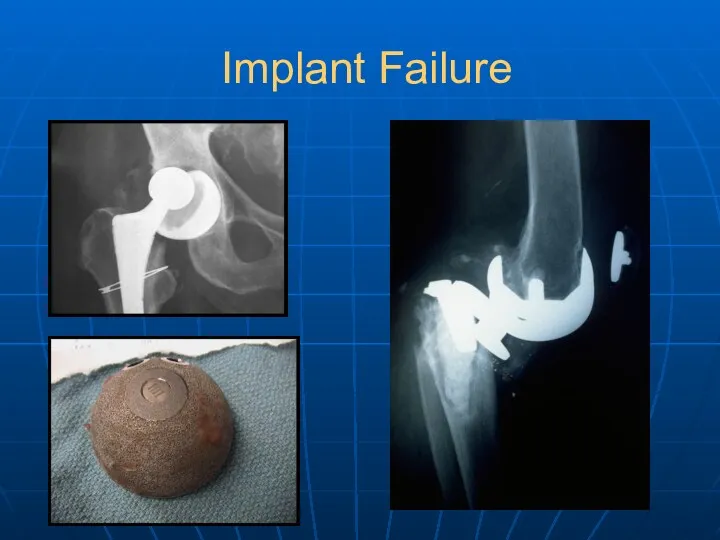
- 36. Implant Failure
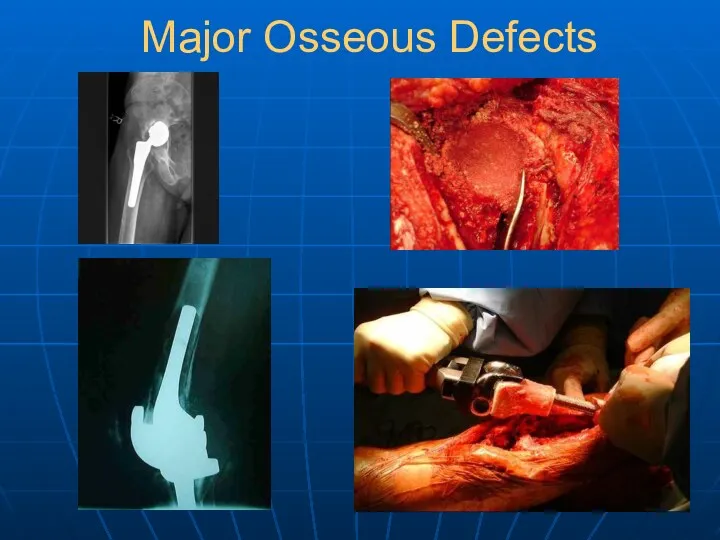
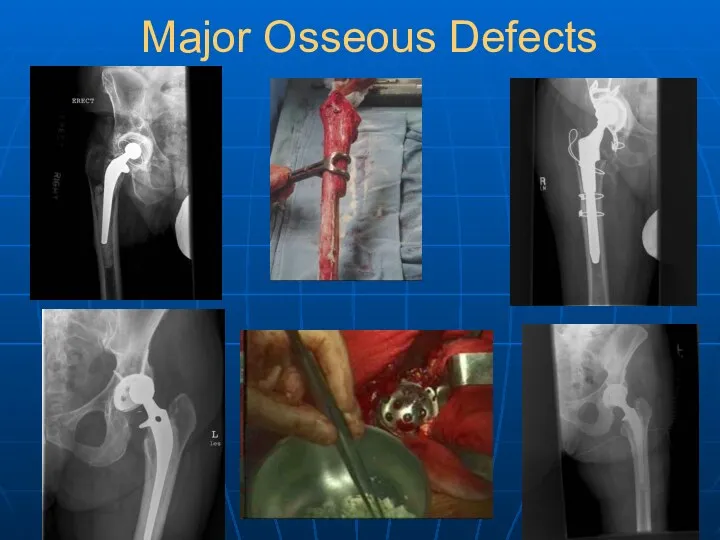
- 37. Major Osseous Defects
- 38. Major Osseous Defects
- 39. Benefits of Revised Codes MEDPAR database Robust source of data for evaluating clinical outcomes, complication rates,
- 40. Benefits of Revised Codes Ability to specify the cause of implant failure Ability to evaluate implant-specific
- 41. Benefits of Revised Codes American Joint Replacement Registry(AJRR) Goals Accurately define the epidemiology of TJR in
- 42. Benefits of Revised Codes Credited with substantially reducing revision rates through early identification of failures Revision
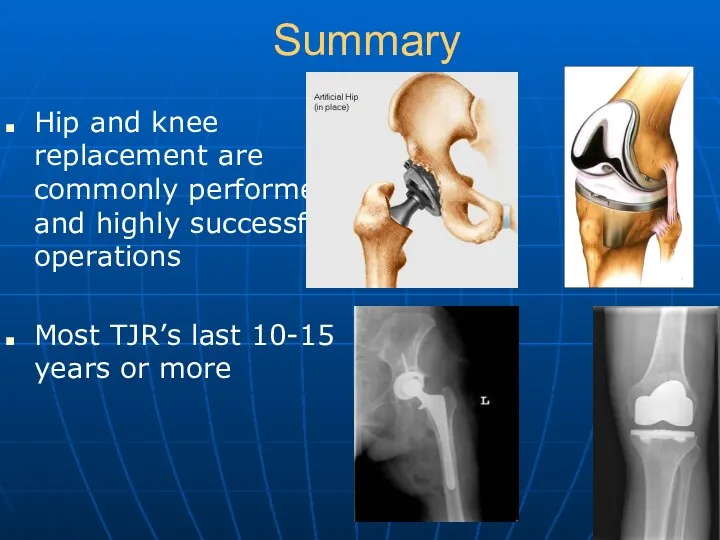
- 43. Summary Hip and knee replacement are commonly performed and highly successful operations Most TJR’s last 10-15
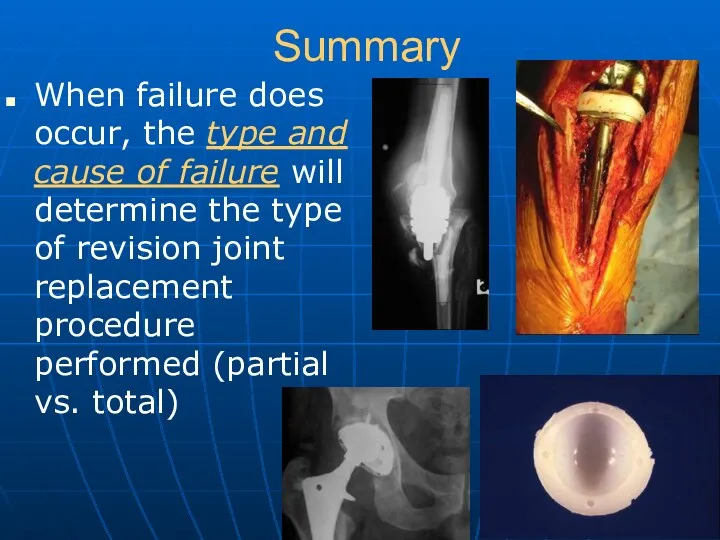
- 44. Summary When failure does occur, the type and cause of failure will determine the type of
- 45. Summary Current ICD-9-CM Diagnosis codes do not provide any information regarding the type or cause of
- 47. Скачать презентацию
















 Фоновые, предраковые заболевания шейки матки
Фоновые, предраковые заболевания шейки матки Косметология. Определение и классификация
Косметология. Определение и классификация Рани. Види ран
Рани. Види ран Профилактика сердечно–сосудистых заболеваний
Профилактика сердечно–сосудистых заболеваний Скрининговые программы по выявлению рака шейки матки и молочных желез, меры профилактики
Скрининговые программы по выявлению рака шейки матки и молочных желез, меры профилактики Наука 2015. Виртуальная книжная выставка
Наука 2015. Виртуальная книжная выставка Лікування цукрового діабету
Лікування цукрового діабету Анатомо-физиологические особенности репродуктивной системы у девочек
Анатомо-физиологические особенности репродуктивной системы у девочек Помощь при укусах и отравлениях
Помощь при укусах и отравлениях Опыт использования системной гипотермии у новорожденных, родившихся в тяжелой асфиксии
Опыт использования системной гипотермии у новорожденных, родившихся в тяжелой асфиксии Российская медицина в русско-японской войне 1904-1905 годов
Российская медицина в русско-японской войне 1904-1905 годов Общие принципы лечения абсцессов и флегмон лица и шеи. Физиотерапия и реабилитация больных
Общие принципы лечения абсцессов и флегмон лица и шеи. Физиотерапия и реабилитация больных Топографическая анатомия и оперативная хирургия тонкой и толстой кишки
Топографическая анатомия и оперативная хирургия тонкой и толстой кишки Өндірістік улардың әсерінің жалпы заңдылықтары
Өндірістік улардың әсерінің жалпы заңдылықтары Предмет и содержание судебной медицины. Процессуальные и организационные основы судебномедицинской экспертизы
Предмет и содержание судебной медицины. Процессуальные и организационные основы судебномедицинской экспертизы Учение об иммунитете
Учение об иммунитете Занятие №5. Костно-мышечная система. Особенности костной системы у детей
Занятие №5. Костно-мышечная система. Особенности костной системы у детей Вирусы гепатита человека. Вирус гепатита В (ВГВ, HВV)
Вирусы гепатита человека. Вирус гепатита В (ВГВ, HВV) ОКИ. Клиника, диагностика, лечение
ОКИ. Клиника, диагностика, лечение Микрофлора полости рта. Состав. Участие в физиологических и патологических процессах полости рта
Микрофлора полости рта. Состав. Участие в физиологических и патологических процессах полости рта Заболевания сальных желёз. Себорея
Заболевания сальных желёз. Себорея Гениталды эндометриоз
Гениталды эндометриоз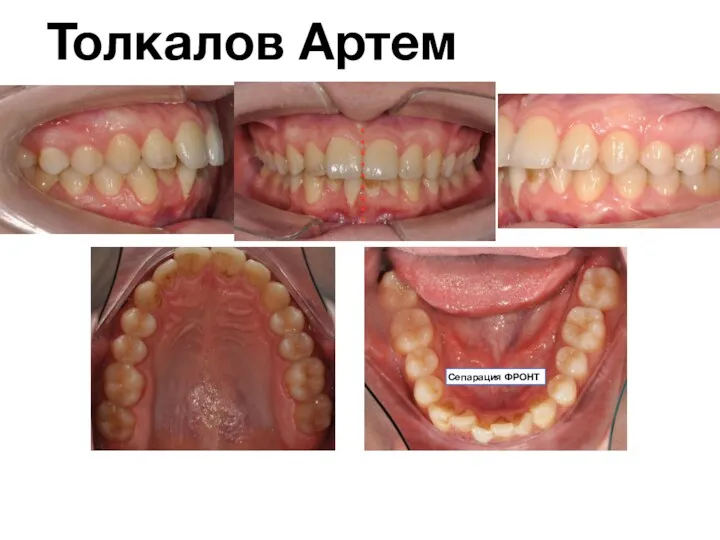 Стоматология. Анализ клинического случая
Стоматология. Анализ клинического случая Геморрагические лихорадки
Геморрагические лихорадки Болезни желчного пузыря, поджелудочной железы. Патология брюшины. Хирургическая патология брюшной полости
Болезни желчного пузыря, поджелудочной железы. Патология брюшины. Хирургическая патология брюшной полости Местные лучевые повреждения
Местные лучевые повреждения Протезирование на имплантатах
Протезирование на имплантатах Жүрек гистологиясы. Жүректің өткізуші жүйесінің морфофункциялық ерекшеліктері
Жүрек гистологиясы. Жүректің өткізуші жүйесінің морфофункциялық ерекшеліктері