Слайд 2

Слайд 3
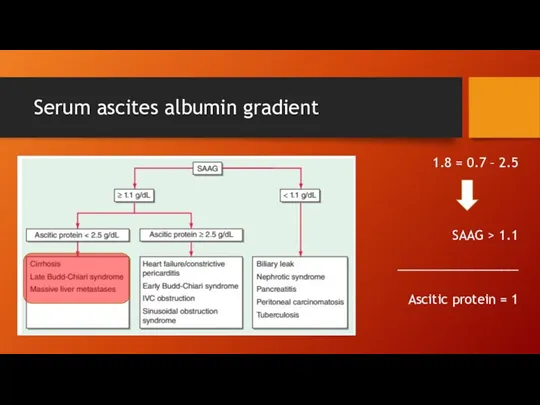
Serum ascites albumin gradient
2.5 – 0.7 = 1.8
SAAG > 1.1
_________________
Ascitic protein
= 1
Слайд 4

Spontaneous bacterial peritonitis
common and severe complication of ascites characterized by spontaneous
infection of the ascitic fluid without an intraabdominal source.
In patients with cirrhosis and ascites severe enough for hospitalization, SBP can occur in up to 30% of individuals and can have a 25% in-hospital mortality rate.
Bacterial translocation is the presumed mechanism for development of SBP, with gut flora traversing the intestine into mesenteric lymph nodes, leading to bacteremia and seeding of the ascitic fluid
The most common organisms are Escherichia coli and other gut bacteria (also enterococci, Strep viridans, Staph aureus…)
The diagnosis of SBP is made when the fluid sample has an absolute neutrophil count >250/μL
Слайд 5

Spontaneous bacterial peritonitis (cont.)
Patients with ascites may present with fever, altered
mental status, elevated white blood cell count, and abdominal pain or discomfort, or they may present without any of these features.
Therefore, it is necessary to have a high degree of clinical suspicion, and peritoneal taps are important for making the diagnosis.
Treatment is with a second-generation cephalosporin, with cefotaxime being the most commonly used antibiotic.
In patients with variceal hemorrhage, the frequency of SBP is significantly
increased, and prophylaxis against SBP is recommended when a patient
presents with upper GI bleeding.
Слайд 6

Hepatorenal syndrome
form of functional renal failure without renal pathology that occurs
in about 10% of patients with advanced cirrhosis or acute liver failure
The diagnosis is made usually in the presence of a large amount of ascites in patients
who have a stepwise progressive increase in creatinine
Type 1 HRS Type 2 HRS
Currently, patients are treated with α-agonist (glypressin) / octreotide and intravenous albumin.
The best therapy for HRS is liver transplantation
Слайд 7

Слайд 8

Слайд 9

Слайд 10

Diagnosis
No specific laboratory or imaging test can be performed to diagnose
irritable bowel syndrome.
Diagnosis involves excluding conditions that produce IBS-like symptoms, and then following a procedure to categorize the patient's symptoms.
Ruling out parasitic infections, lactose intolerance, small intestinal bacterial overgrowth, and celiac disease is recommended for all patients before a diagnosis of irritable bowel syndrome is made.
In patients over 50 years old, they are recommended to undergo a screening colonoscopy
Слайд 11

Слайд 12

Слайд 13
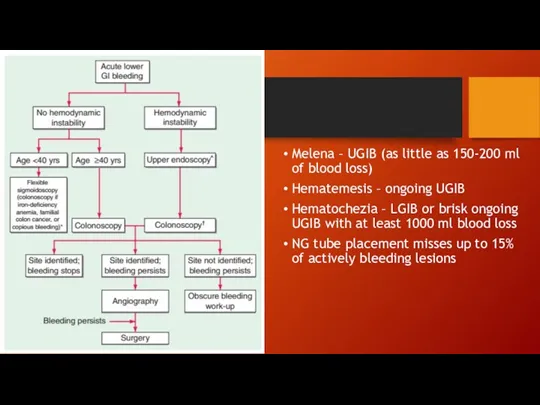
Melena – UGIB (as little as 150-200 ml of blood loss)
Hematemesis
– ongoing UGIB
Hematochezia – LGIB or brisk ongoing UGIB with at least 1000 ml blood loss
NG tube placement misses up to 15% of actively bleeding lesions
Слайд 14

Слайд 15
Слайд 16
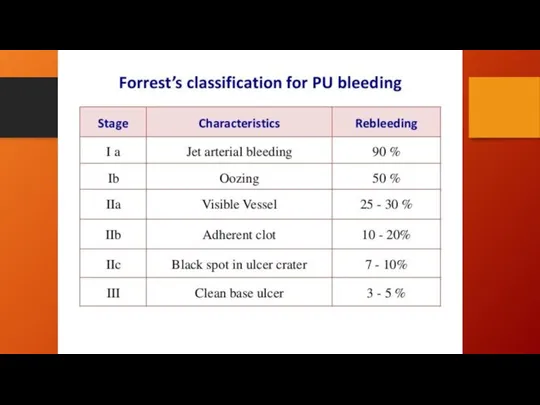

Слайд 17
Слайд 18
Слайд 19
Слайд 20
Слайд 21

Слайд 22

Слайд 23
Слайд 24

Слайд 25

Слайд 26

Dyspepsia in patient younger than 50 yo w/o alarm features
Anemia
Dysphagia
Odynophagia
Weight loss
Vomiting
FH
of UGI malignancy
PH of PUD, gastric surgery or GI malignancy
Abdominal mass / LAD on exam
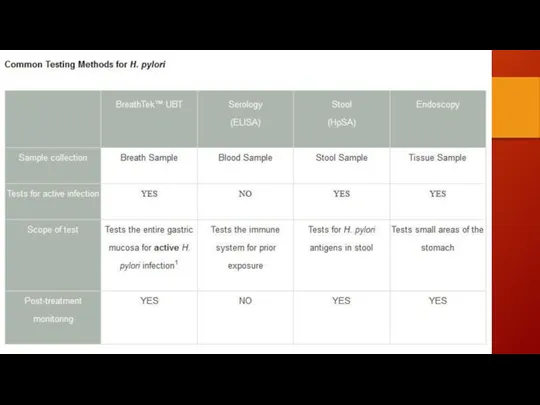
Test for H.pylori
(+) (-)
Eradication PPI trial
Слайд 27
Слайд 28
Слайд 29

Слайд 30

Слайд 31
Слайд 32

Слайд 33
Слайд 34


































 Современные требования к назначению, оформлению рецептов, требований на ЛП и МИ и их отпуску из аптечных организаций
Современные требования к назначению, оформлению рецептов, требований на ЛП и МИ и их отпуску из аптечных организаций Специфическая (антидотная) фармакотерапия острых отравлений
Специфическая (антидотная) фармакотерапия острых отравлений Репродуктивное здоровье подростка
Репродуктивное здоровье подростка Воздействие наноматериалов на организм человека. Концепция токсикологических исследований
Воздействие наноматериалов на организм человека. Концепция токсикологических исследований Физиология половой дифференцировки и возрастные изменения функций половых желез
Физиология половой дифференцировки и возрастные изменения функций половых желез Медицинский отряд специального назначения
Медицинский отряд специального назначения Хирургические инфекции
Хирургические инфекции Будь здоров
Будь здоров Методы обследования больного - пальпация, перкуссия. Методы исследования и симптоматология заболеваний органов дыхания
Методы обследования больного - пальпация, перкуссия. Методы исследования и симптоматология заболеваний органов дыхания Биоэтика: возникновение, структура, принципы
Биоэтика: возникновение, структура, принципы Аса қауіпті аурулар
Аса қауіпті аурулар Аяқ қол хирургиялық аурулары,туа біткен ақаулары және жарақаттары
Аяқ қол хирургиялық аурулары,туа біткен ақаулары және жарақаттары Радионуклидная диагностика в кардиологии
Радионуклидная диагностика в кардиологии Психические расстройства вследствие органического поражения головного мозга
Психические расстройства вследствие органического поражения головного мозга Организация работы специализированных и линйных бригад скорой медицинской помощи
Организация работы специализированных и линйных бригад скорой медицинской помощи Гигиенические требования к условиям и режиму пребывания в детских и подростковых учреждениях
Гигиенические требования к условиям и режиму пребывания в детских и подростковых учреждениях Симптоматические гипертонии в амбулаторной практике
Симптоматические гипертонии в амбулаторной практике Новый коронавирус 2019- nCоV
Новый коронавирус 2019- nCоV Вскармливание детей грудного возраста
Вскармливание детей грудного возраста Врачебная этика Френсиса Бэкона
Врачебная этика Френсиса Бэкона Лікування хворих на цукровий діабет
Лікування хворих на цукровий діабет Организация и тактика медицинской службы (ОТМС)
Организация и тактика медицинской службы (ОТМС) Неотложная терапия анафилактических реакций
Неотложная терапия анафилактических реакций Правила парентерального введения лекарственных средств. Сестринское дело
Правила парентерального введения лекарственных средств. Сестринское дело Частная травматология. Повреждения тупыми предметами
Частная травматология. Повреждения тупыми предметами Инструкция для медицинского применения лекарств и вопросы безопасности
Инструкция для медицинского применения лекарств и вопросы безопасности Средства, действующие на эфферентную иннервацию
Средства, действующие на эфферентную иннервацию Опухоли почек
Опухоли почек