Содержание
- 2. Introduction Endodontics is the specialty of dentistry that manages the prevention, diagnosis, and treatment of the
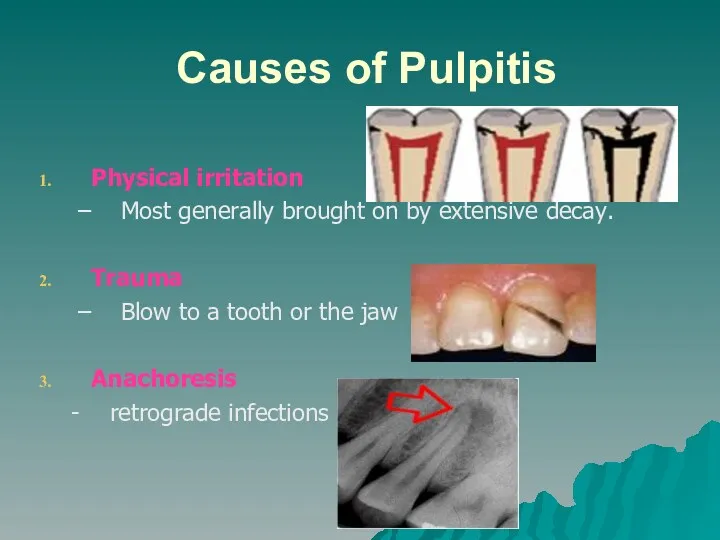
- 3. Causes of Pulpitis Physical irritation Most generally brought on by extensive decay. Trauma Blow to a
- 4. Signs and Symptoms Pain when biting down Pain when chewing Sensitivity with hot or cold beverages
- 5. Endodontic Diagnosis Subjective examination Chief complaint Character and duration of pain Painful stimuli Sensitivity to biting
- 6. Important questions? What do you think the problem is? Does it hurt to hot or cold?
- 7. Objective examination Extent of decay Periodontal conditions surrounding the tooth in question Presence of an extensive
- 8. Challenges in diagnosis of pulpitis Referred pain & the lack of proprioceptors in the pulp localizing
- 9. Diagnostic Tests Percussion Palpation Thermal Electrical Radiographs
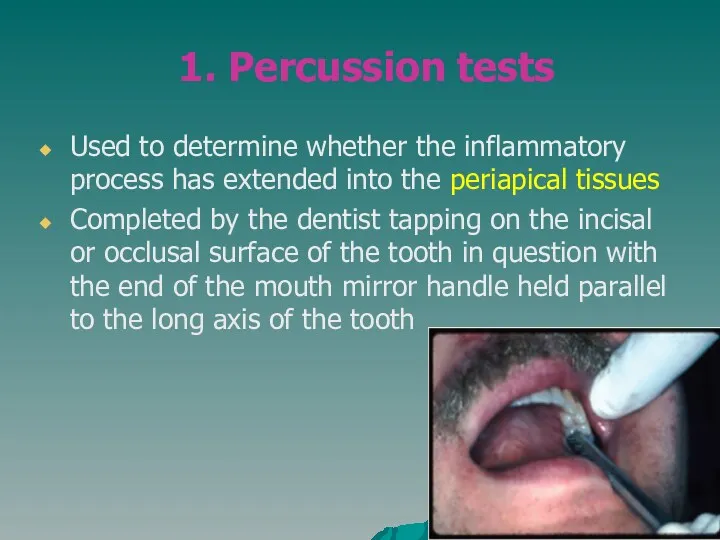
- 10. 1. Percussion tests Used to determine whether the inflammatory process has extended into the periapical tissues
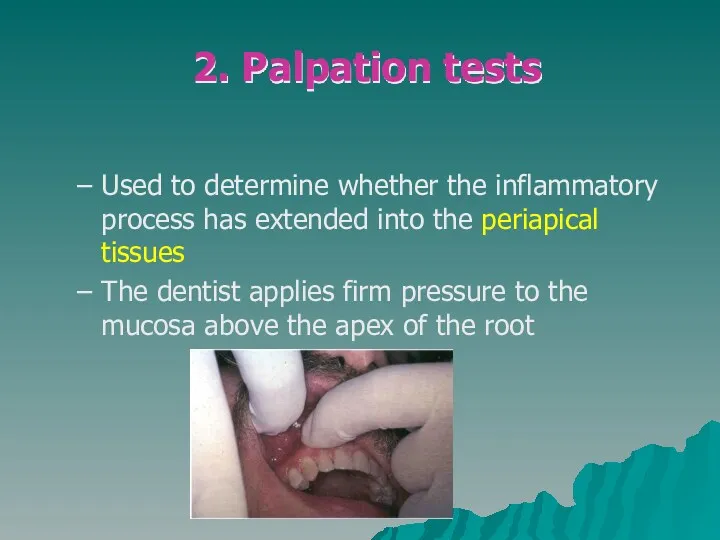
- 11. Used to determine whether the inflammatory process has extended into the periapical tissues The dentist applies
- 12. 3. Thermal sensitivity Necrotic pulp will not respond to cold or hot Cold test Ice, dry
- 13. Evaluation of thermal test results 4 distinct responses: No response non-vital pulp or false negative Mild
- 15. Causes of false positives/negative Calcified canals Immature apex – usually seen in young patients Trauma Premedication
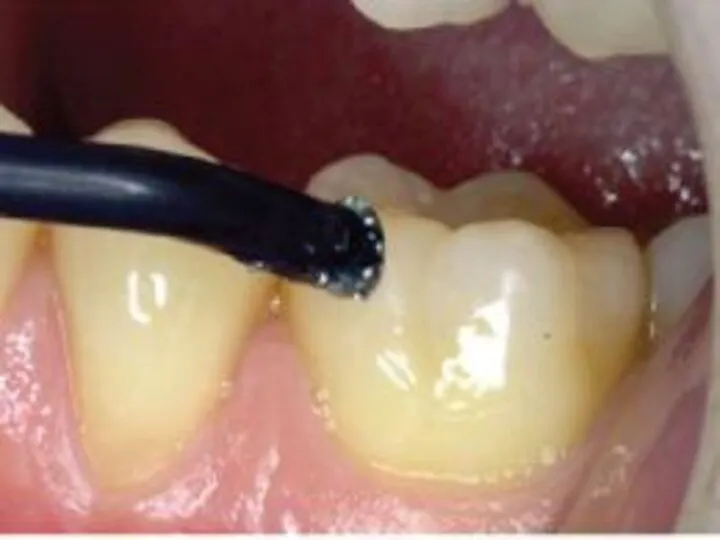
- 16. 4. Electric pulp testing Delivers a small electrical stimulus to the pulp Factors that may influence
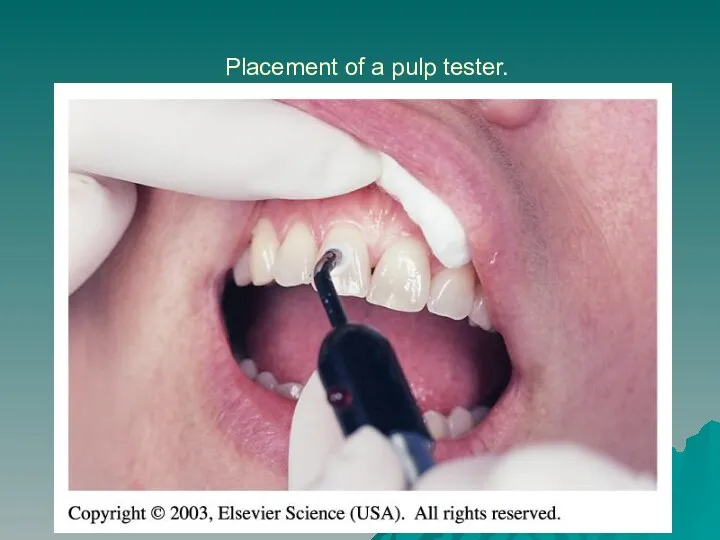
- 17. Placement of a pulp tester.
- 19. 5. Radiographs Pre-operative radiograph Invaluable diagnostic tool Periapical radiolucency Widening of PDL Deep caries Resorption Pulp
- 20. Requirements of Endodontic Films Show 4-5 mm beyond the apex of the tooth and the surrounding
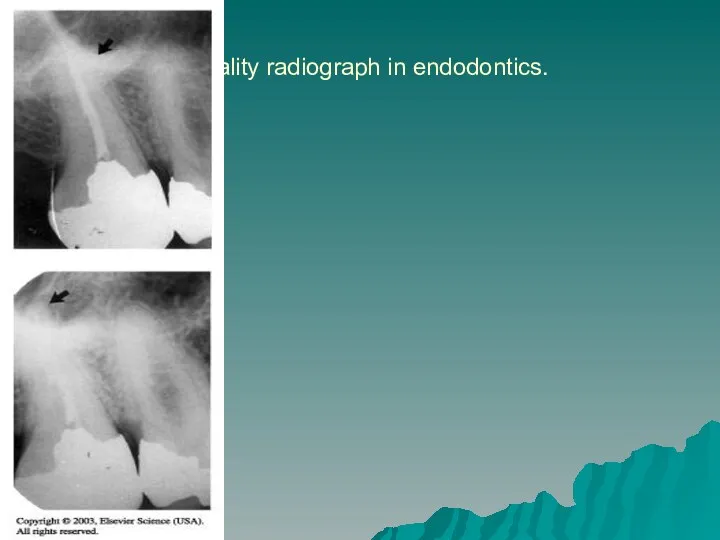
- 21. Quality radiograph in endodontics.
- 22. Diagnostic Conclusions Normal pulp Pulpitis
- 23. Normal pulp There are no subjective symptoms or objective signs. The pulp responds normally to sensory
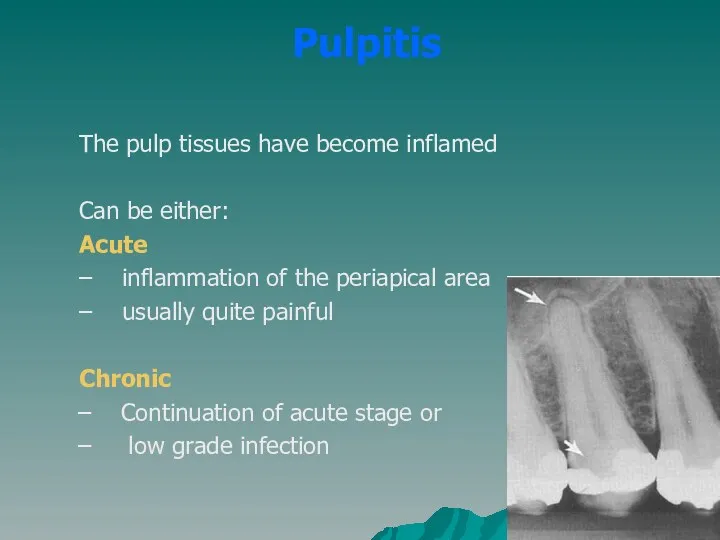
- 24. Pulpitis The pulp tissues have become inflamed Can be either: Acute – inflammation of the periapical
- 25. Acute Pulpitis mainly occurs in children teeth and adolescent pain is more pronounced than in chronic
- 26. Symptoms and Signs of acute pulpitis The pain not localized in the affected tooth is constant
- 28. Forms of acute pulpitis 1. Form of purulent acute where the pulp is totally inflammed 2.
- 29. Chronic Pulpitis Reversible Irreversible
- 30. Reversible pulpitis The pulp is irritated, and the patient is experiencing pain to thermal stimuli Sharp
- 31. Irreversible pulpitis The tooth will display symptoms of lingering pain pain occurs spontaneously or lingers minutes
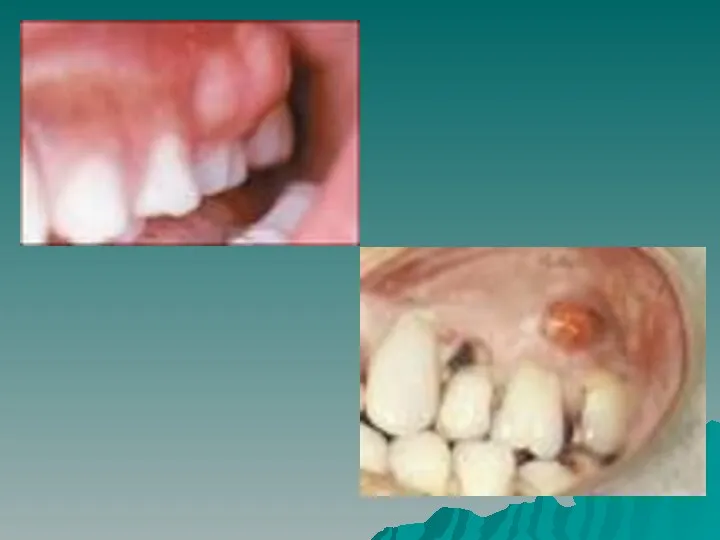
- 32. Periradicular abscess An inflammatory reaction to pulpal infection that can be chronic or have rapid onset
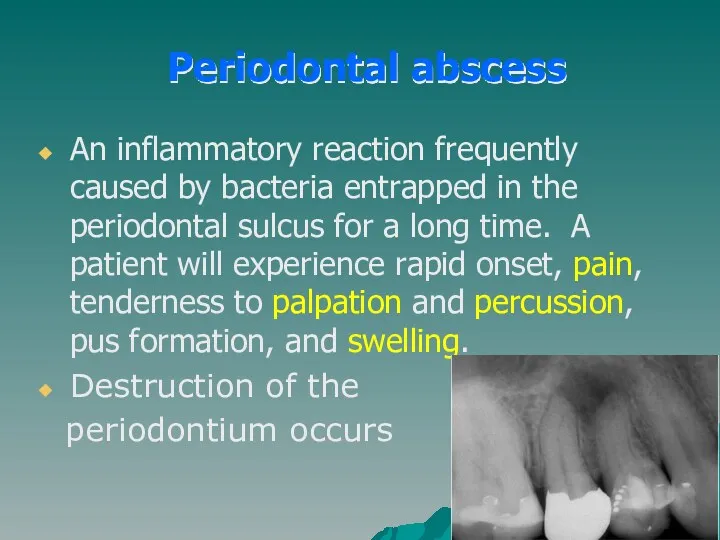
- 34. An inflammatory reaction frequently caused by bacteria entrapped in the periodontal sulcus for a long time.
- 36. Periradicular cyst A cyst that develops at or near the root of a necrotic pulp. These
- 37. Pulp fibrosis The decrease of living cells within the pulp causing fibrous tissue to take over
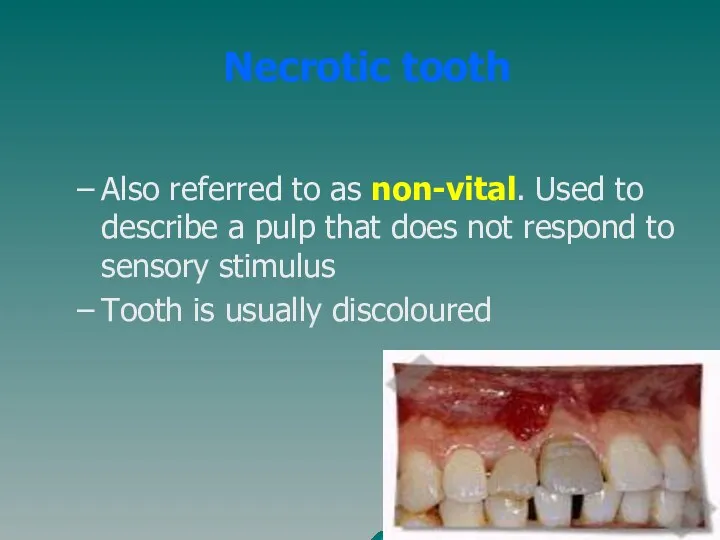
- 38. Necrotic tooth Also referred to as non-vital. Used to describe a pulp that does not respond
- 39. Plan of Treatment Depends widely on the diagnosis
- 40. Simple plan of treatment Visit 1: Medical history History of the tooth Access cavity Place rubberdam
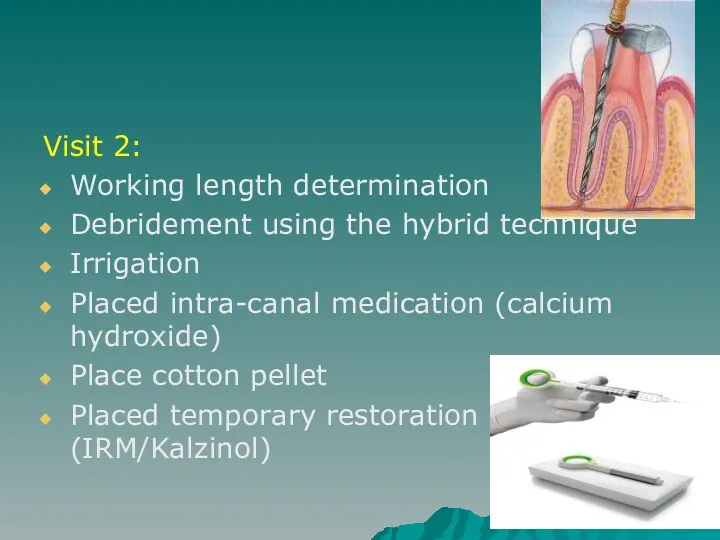
- 41. Visit 2: Working length determination Debridement using the hybrid technique Irrigation Placed intra-canal medication (calcium hydroxide)
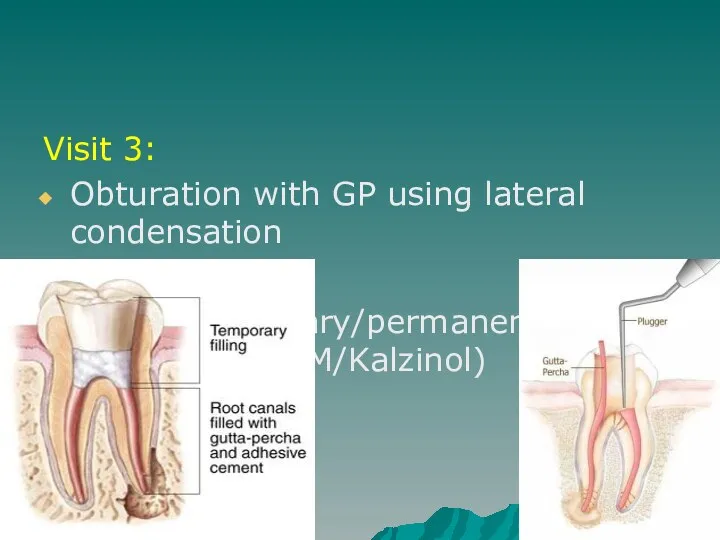
- 42. Visit 3: Obturation with GP using lateral condensation Placed temporary/permanent restoration (IRM/Kalzinol)
- 43. Referral To appropriate discipline
- 44. Remember Access cavity shapes: Anterior – inverted triangle Premolars – round Molars – rhomboid Always use
- 45. Contraindications for RCT Caries extending beyond bone level Rubberdam cannot be placed Crown of tooth cannot
- 46. Inter & cross-departmental diagnosis Mobile teeth Teeth associated with severe periodontal problems Confusion between TMJ dysfunctional
- 48. Скачать презентацию
































 Депрессия в пожилом возрасте
Депрессия в пожилом возрасте Рак ободочной кишки (C-r coli)
Рак ободочной кишки (C-r coli) Проблема здоровья людей: глобальный аспект
Проблема здоровья людей: глобальный аспект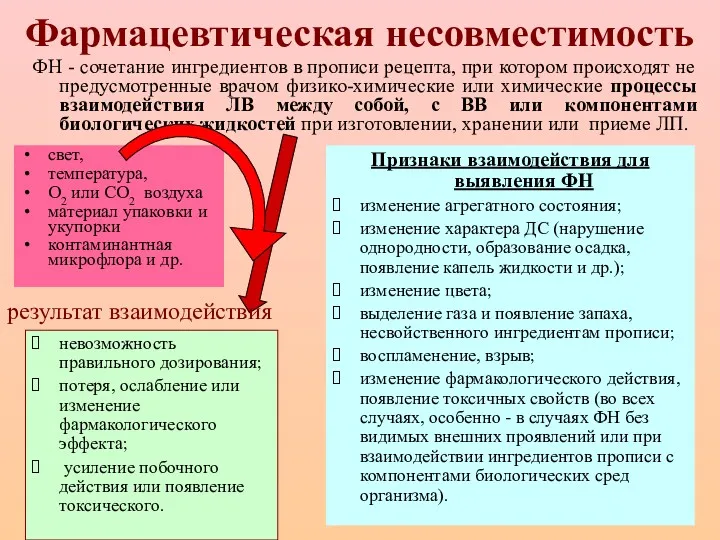 Фармацевтическая несовместимость
Фармацевтическая несовместимость Злокачественные новообразования желудка
Злокачественные новообразования желудка Средства индивидуальной защиты (противочумные костюмы I, II, III, IV типа)
Средства индивидуальной защиты (противочумные костюмы I, II, III, IV типа) Острая ревматическая лихорадка
Острая ревматическая лихорадка Дәрігер мен науқас арасында туындайтын шиеленіс
Дәрігер мен науқас арасында туындайтын шиеленіс Алькогольдің адам организміне зияны
Алькогольдің адам организміне зияны Определение группы крови по системе АВ0 моноклональными антителами (цоликлонами)
Определение группы крови по системе АВ0 моноклональными антителами (цоликлонами) Инфекционные заболевания и беременность
Инфекционные заболевания и беременность Регуляция кровообращения
Регуляция кровообращения Неспецифическая хирургическая инфекция
Неспецифическая хирургическая инфекция Деонтология в хирургии
Деонтология в хирургии Генетика и наследственные заболевания человека
Генетика и наследственные заболевания человека Виды частичных съемных протезов. Способы их фиксации
Виды частичных съемных протезов. Способы их фиксации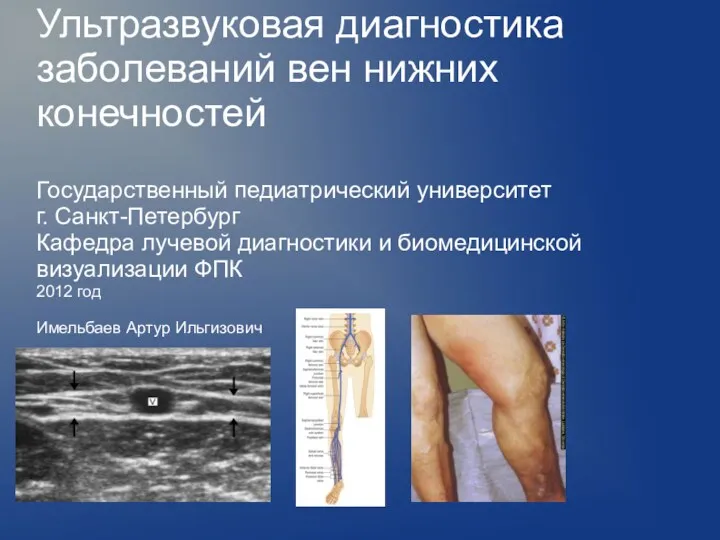 Ультразвуковая диагностика заболеваний вен нижних конечностей
Ультразвуковая диагностика заболеваний вен нижних конечностей Витамины. (Часть 2)
Витамины. (Часть 2) Психотерапевтический метод музыкотерапия
Психотерапевтический метод музыкотерапия Лечение туберкулеза у детей и подростков
Лечение туберкулеза у детей и подростков DSD-template
DSD-template Отбасын жоспарлау сұрақтары. Контрацепция. Әйелдің репродуктивті денсаулығын қорғау
Отбасын жоспарлау сұрақтары. Контрацепция. Әйелдің репродуктивті денсаулығын қорғау Гемолитическая болезнь новорожденных
Гемолитическая болезнь новорожденных Профилактика, диагностика, и оптимизация лечения маргинальной резорбции костной ткани
Профилактика, диагностика, и оптимизация лечения маргинальной резорбции костной ткани Закономерности распределения лекарственных веществ в организме мелких домашних животных
Закономерности распределения лекарственных веществ в организме мелких домашних животных Врожденная дисфункция коры надпочечников
Врожденная дисфункция коры надпочечников Тіс ішінара болмағанда немесе түгел болмағанда қолданылатын ортопедиялық ем. Операциялық және қалпына келтіретін дентистрия
Тіс ішінара болмағанда немесе түгел болмағанда қолданылатын ортопедиялық ем. Операциялық және қалпына келтіретін дентистрия Жасына сәйкес екпе алмаған балаға жеке егу күнтізбесін құрастыру
Жасына сәйкес екпе алмаған балаға жеке егу күнтізбесін құрастыру